Computing technologies for healthcare

The School pioneers healthcare technologies that target applications in computational biology, intelligent social agents, decision support tools, brain computer interfaces and health monitoring. Statistical machine learning approaches explain cancer and virus evolution, provide decision support based on Electronic Health Records and develop intelligent agents that sense human neurophysiology and provide support in mental and psychiatric disorders including dementia, autism and depression. The School has more than 30 years’ experience in information retrieval that relates to privacy issues and fair-representations in sensitive data. The School is also involved in building the next generation of quantum imaging technology for monitoring of Wellbeing and disease.
There is a strong culture of inter-disciplinary research and training via several links that include Glasgow Polyomics, Institute of Cancer Sciences, MRC Centre for Virus Research, Glasgow Precision Oncology Laboratory, Robertson Centre for Biostatistics, the Institute of Neuroscience and Psychology, the Adam Smith Business School, the School of Critical Studies, the School of Engineering, the Scottish Graduate School of the Social Sciences and the School of Physics and Astronomy.
Theme Lead: Dr Stephen Lindsay
Current Projects
The Social AI CDT 2019-2027. EPSRC
Prof Alessandro Vinciarelli, Prof Iadh Ounis, Dr Mary-Ellen Foster
The Social AI CDT, based at the University of Glasgow, is a collaboration between the School of Computing Science, the School of Psychology & Neuroscience, the Adam Smith Business School, the School of Critical Studies, the School of Engineering, the Scottish Graduate School of the Social Sciences and 17 industrial partners to 1) outline principles and laws that govern social interactions between human and artificial agents – both embodied and virtual – at the level of cognitive, behavioural and physiological phenomena 2) to improve the impact of artificial agents through their integration into wider and more complex technological systems and infrastructures 3) to develop technological approaches – informed by the principles and laws outlined in 1 – that allow artificial agents to act as believable and effective partners in social interactions involving human users and 4)to investigate the human response to socially intelligent artificial agents in everyday life.
Beyond One Solution in Combinatorial Optimisation 2021-2026. EPSRC
Dr. Kitty Meeks (PI), Dr. Jessica Enright, Dr. Craig Anderson, Dr. Bhautesh Jani
A £1.36 million EPSRC fellowship which will develop new methods for understanding the space of all "good" solutions to optimisation problems - such as clustering - rather than searching for a single "best" solution, and apply these techniques to address challenges in digital health. Specific applications include treatments for heart failure, diagnosis of endometriosis, targeted cancer screening, and the identification of optimal interventions for infectious disease control.
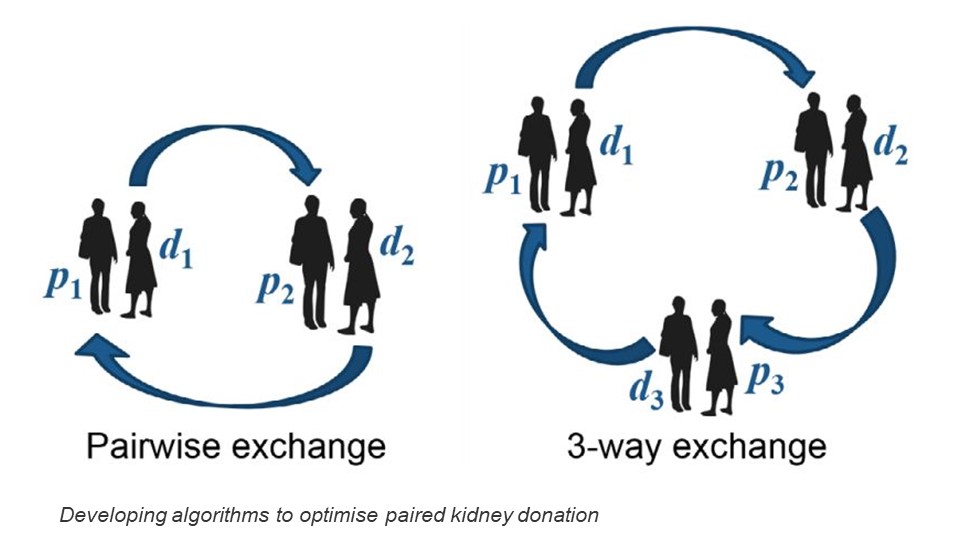
KidneyAlgo: New Algorithms for UK and International Kidney Exchange 2023-2025. EPSRC
Prof David Manlove
This collaborative project with Durham University involves developing new algorithms and software for the UK Living Kidney Sharing Scheme (UKLKSS) and for other kidney exchange programmes (KEPs) around Europe. The new algorithms will allow for more complex exchange structures, larger pools and different optimality objectives within the UKLKSS. For international kidney exchange programmes that involve collaboration between multiple countries, the algorithms will ensure fairness and stability, incentivising countries to participate in a shared KEP.
Privacy-Preserved Human Motion Analysis for Healthcare Applications 2022-2025. EPSRC
Dr. Fani Deligianni
A new investigator award, which will develop artificial intelligence algorithms for human motion analysis in healthcare applications that preserve users' privacy
Quantum Imaging for Monitoring of Wellbeing & Disease in Communities 2020-2025. EPSRC
Prof. Roderick Murray-Smith (Co-I)
A multi-million project on how quantum imaging will enable remote detection and monitoring of parameters such as gait, macro and micro-movements, blood flow, heart rate and potentially even brain function. When combined with data-driven models, will allow to both monitor health and the onset of non-communicable diseases (NCDs) but also recovery from NCDs or surgery with personalised and continuously updated re-habilitation programmes.
Safe Information Extraction from Patient Histories 2023-2025. EPSRC
Dr. Graham McDonald, Dr. Jake Lever and Prof. Iadh Ounis
A New Horizons project to develop methods for extracting information from patient records while maintaining patient privacy. Information in the free text of medical records can be key to important medical discoveries but high-quality annotated text is needed for effective information extraction. This project will research the use of synthetic medical records to create text annotations which don't risk leaking sensitive information.
Digitalisation of livestock data to improve veterinary public health 2021-2024. NordForsk
Dr. Jessica Enright
The DigiVet project will study how livestock data is currently used across the partner nations, and how technology, training, and regulatory frameworks might provide societal benefit by improving the public-interest uses of these data.
Personalised Acceptance and Commitment Therapy (PACT) for Parkinson's Disease 2023-2024. ParkinsonsUK
Dr Siomone Stumpf
Living with Parkinson’s disease presents daily challenges, which can affect a person’s wellbeing. Face-to-face talking therapies are effective at improving wellbeing but can be time-consuming and difficult to access. The COVID-19 pandemic has reduced access to face-to-face support and expanded our digital world. Digital applications on smartphones and tablets are an effective way of delivering psychological support. The aim of this study is to develop and test a digital application which provides brief daily support for psychological wellbeing based on the talking therapy Acceptance and Commitment Therapy (ACT)
Pancreatic cancer AI for genomics and personalized Medicine 2021-2024. Horizon 2020
Dr Ke Yuan
PANCAIM will combine genomics and imaging phenomics using AI to generate breakthrough knowledge to increase understanding of PDAC biology and patient stratification. It will develop trusted impactful AI applications for regular clinical use to help clinical decision-makers to give the right treatment to the right patients at the right time, and at the right cost and improve treatment outcomes of PDAC patients.
Multilayer Algorithmics to Leverage Graph Structure (MultilayerALGS) 2020-2023. EPSRC
Dr. Kitty Meeks, Dr. Jessica Enright, Prof Duncan Lee, Dr. Mark Wong, Dr. Heng Guo (University of Edinburgh)
A broad project about novel algorithmic techniques to handle network datasets involving qualitatively different types of edges (for example, physical and online contact in a social network) involves two application case studies related to healthcare: finding optimal epidemiological interventions when a disease spreads in a multi-layer networks, and identifying spatial patterns in disease risk for non-communicable diseases.
Using AI-Enhanced Social Robots to Improve Children's Healthcare Experiences 2020-2023. ESRC/SSHRC
Dr Mary-Ellen Foster
In this project, we aim to address this limitation by developing and evaluating a clinically relevant and responsive AI-enhanced social robot. We believe that interaction with a robust, adaptive, socially intelligent robot can effectively distract children during painful clinical procedures, thereby reducing pain and distress.
Academic Staff
- Dr. Christos Anagnostopoulos, (Pervasive and Distributed Intelligence)
- Dr. Matthew Barr, (Video games, well-being and mental health)
- Prof. Stephen Brewster, (Human Computer Interactions technologies for mental disorders)
- Dr. Kevin Bryson, (Bioinformatics and histopathology image analysis)
- Dr. Mathieu Chollet, (Virtual Social Interactions)
- Dr Hang Dai, (Computer vision and meidical imaging)
- Dr. Fani Deligianni, (Decision support systems, analysis of neurophysiological data)
- Dr. Xianghua Ding, (Patient-Provider Communication, Co-Production in Healthcare, and Health Tracking Technologies)
- Dr. Jessica Enright, (Graph theory in epidemiology research)
- Dr. Mary Ellen Foster, (Building artificial characters that interact naturally with people)
- Dr Ali Gooya, (Computer vision and medical imaging)
- Dr Edmond Ho, (Analyzing human data captured from visual sensors)
- Dr. Jake Lever, (Information Extraction and Retrieval in Biomedical Applications)
- Dr Emma Li, (Human-robot partnerships for health and social care)
- Dr. Stephen Lindsay, (Digital healthcare and co-design)
- Dr. Sean MacAvanney, ()
- Dr. Craig MacDonald, (Information Retrieval)
- Dr. Marwa Mahmoud, (Multimodal behaviour analytics)
- Prof. David Manlove, (Matching problems in the field of algorithms and complexity)
- Dr. Zaiqiao Meng, (Biomedical knowledge graph and natural language processing)
- Prof. Iadh Ounis, (Information Retrieval)
- Dr. William Pettersson, (Complexity theory, Theoretical efficiency of an algorithm)
- Dr. Kitty Meeks, (Graph theory in epidemiology research, clustering algorithms)
- Dr. Lito Michala (Internet of Things)
- Prof. Roderick Murray-Smith, (Inference, Dynamics and Interaction)
- Dr. Jose Cano Reyes, (Computer Architecture, Edge Computing, Deep Learning)
- Dr. Simone Stumpf, (Responsible & Interactive Artificial Intelligence)
- Prof. Alessandro Vinciarelli, (Computational Social Intelligence)
- Dr John Williamson, (Human Computer Interfaces in healthcare applications)
- Dr. Ke Yuan (Bioinformatics and cancer research)
Research Students
Asking questions about medical images. 2020-2024. Canon Medical Systems
Maciej Pajak, Dr. Fani Deligianni, Dr. Jeff Dalton
This project focuses on a range of methodological approaches in computer vision and natural language processing, which collectively support answering questions about 2D and 3D radiology images.
PhD Scholarship on Applying machine learning models to genome data to understand the evolution of drug resistance from virus to cancer evolution. 2020-2024. MRC Precision Medicine DTP
Dr. Ke Yuan.
PhD Scholarship on A Network Clustering Approach to Endometriosis Diagnosis. 2019-2023. MRC Precision Medicine DTP.
Dr. Kitty Meeks, Dr Craig Anderson
EngD project on multi-modal and self-supervised machine learning for medical image analysis. 2018-2021. Canon Medical Research
Dr. Bjorn Jensen
PhD Placement Mobility grant on ‘Endoscopic Surgery Image Enhancement’ 2020-2021. Newton Bhabha Fund
Dr. Jose Cano Reyes
This project aims to design hardware architectures to remove unwanted distortions in the input pixels due to surgical smoke or fog particles for real-time operations.
Past Projects
Closed-Loop Data Science for Complex, Computationally- and Data-Intensive Analytics
Prof. Roderick Murray-Smith, Dr. Craig Macdonald, Dr. Nikos Darmos, Prof. Iadh Iounis, Dr. Ke Yuan, Dr. Simon Rogers, Dr. Christos Anagnostopoulos, Dr. Bjorn Jensen, Dr. John Williamson
A multi-million project on ‘Closed-loop Data Science’ applied in several areas including personalisation of hearing aids and analysis of cancer data.
TREC Precision Medicine campaign 2020-2022.UFMG (Brazil)
Dr Craig Macdonald and Prof. Iadh Ounis
Developing search technologies for precision medicine and biomedical text. It come 2nd among 25 groups worldwide in the TREC Precision Medicine campaign in November (NIST, USA). The developed system was also one of the best performing among 50 participating groups in the TREC COVID campaign to automatically distil information from published articles as the pandemic progressed.
African COVID-19 preparedness (AFRICO19) 2020-2022. The Wellcome Trust
Dr. Ke Yuan (Co-I)
This project will enhance capacity to understand SARS-CoV-2/hCoV-19 infection in three regions of Africa (Kenya, The Gambia and Uganda) and globally.
UK Living Kidney Sharing Scheme 2016-2021. CA15210 - European Network for Collaboration on Kidney Exchange Programmes, European Cooperation in Science and Technology (COST)
Prof. David Manlove Dr. William Pettersson
Over 1200 kidney transplants identified by the algorithms developed at Glasgow that match patients and donors for the UK Living Kidney Sharing Scheme have proceeded to surgery. This is estimated to have saved the NHS around £90M over the period 2008-2030, taking into account the cost of the surgery versus the savings made by releasing a patient from long-term dialysis. Read more in these two articles: ‘How Operational Research Helps Kidney Patients in the UK’ and ‘Algorithms for Kidney Donation’
iCaird - the Industrial Centre for Artificial Intelligence Research in Digital Diagnostics 2018 – 2021. Innovate UK
Prof. Rod Murray-Smith, Prof. Muffy Calder, Dr. Bjorn Sand Jensen and Dr. John Williamson
The Industrial Centre for Artificial Intelligence Research in Digital Diagnostics was announced on the 6th of November 2018 as one of five successful bids to the UK Governments UKRI Industrial Strategy Challenge Fund (ISCF). It brings together a pan-Scotland collaboration of 15 founding partners from across industry, the NHS, and academia; including four current actively engaged SMEs. Industry leadership is provided by Canon Medical Research Europe (radiology) and Royal Philips (digital pathology). iCAIRD was awarded £10m in ISCF funding by Innovate UK, while partner companies Canon Medical Research Europe Ltd, Royal Philips and SMEs are collectively providing £6M of additional supportive funding. Today iCAIRD has more than 30 active partner companies, with over 30 current research projects across radiology and pathology
A Robot Training Buddy for Adults with ASD 2017-2021. EPSRC
Prof. Alessandro Vinciarelli and Dr. Mary Ellen Foster
This project promotes collaboration with the Scottish Autism Centre and it aims to teach social skills to autistic adults via robots.
Funded by EPSRC.
A high-content platform for cellular mechanobiology in cancer research 2018-2021. CRUK
Dr Bjorn Jensen
The project aims to develop technological solutions of handling wearable data based on deep learning to address ethical and data privacy considerations of patients and their social cycle.
Human Motion Analysis – Agency, Negotiation and Legibility in Data Handling 2020-2021. Human Data Interaction EPSRC Network
Dr. Fani Deligianni
Fast multi-shot epidemic interventions for post lockdown Covid-19 mitigation: Open-loop mitigation strategies 2020. EPSRC funded project, EP/V018450/1.
Prof. Rod Murray-Smith
The objective of this project is to design and validate new exit-strategies from the current lockdown policy that actively suppress COVID-19, while allowing significant economic activity. Currently proposed exit-strategies suggest that intermittent lockdowns, in addition to contact tracing, masking, and other measures, may be necessary until an effective vaccine is found. Our suggestion is to develop periodic open-loop lockdown strategies over short timescales. Such policies will help suppressing the virus and allow predictable periodic periods of lockdown, thereby facilitating economic activity. The policies will be validated on advanced, realistic epidemiological mathematical models and data, and will be developed for national and international compartmental scenario
Technology Enabled Mental Health for Young People 2016-2020.H2020 International Training Network
Prof. Steven Brewster
The network aims to design, develop and evaluate novel technologies to enable mental health services that are effective, affordable and accessible for young people.
Royal Society of Edinburgh/Scottish Enterprise Entrepreneurial Fellowship CH12 on Clydescope Health 2018-2019
Dr Anna Lito Michala
This project focused on developing an automated mix and infusion system that monitored hypoglycaemia, prepared the glucagon and injected just in time to avoid loss of consciousness. The IoT device was edge processing information locally and only connected to a smartphone app to securely inform careers if intervention was required and alarm patients to take further action.
Dr. Kitty Meeks, Dr. Craig Anderson
SAM: Automated Attachment Analysis Using the School Attachment Monitor 2015-2018. EPSRC
Prof. Steven Brewster, and Prof Alessandro Vinciarelli
Analysis of attachment patterns in school age children with collaboration with the Adverse Childhood Experiences Centre.
MoreGrasp - 2015-2018. EC Horizon2020 project
Prof. Roderick Murray-Smith
Final Demo video. The aim of the MoreGrasp project is to develop a non-invasive, multi-adaptive, multimodal user interface including a brain-computer interface (BCI) for intuitive control of a semi-autonomous motor and sensory grasp neuroprosthesis supporting individuals with high spinal cord injury in everyday activities.
How to join
Funded PhD Opportunities on healthcare applications are provided via the following main routes:
Visit University of Glasgow vacancies for job opportunities.
Upcoming events
There are currently no upcoming events
Past events
AI and Health: Harnessing Norwegian Data for Personalized and Predictive Care (19 May, 2025)
Speaker: Prof. Kerstin Bach
Collaborative Opportunities with Singapore Institute of Technology (29 November, 2024)
Speaker: Ng Pai Chet
Join us for a special two-part seminar that combines a seminar on 'Mobile Hyperspectral Imaging for Democratized Skin Analysis' with exciting international collaboration opportunities.
Part 1: Research Presentation "Mobile Hyperspectral Imaging for Democratized Skin Analysis" by Dr. Ng Pai Chet. The presentation will explore how everyday selfies can be transformed into powerful tools for skin analysis through hyperspectral reconstruction and AI. Using the novel Hyper-Skin dataset of 330 hyperspectral cubes, we'll demonstrate how deep learning can enable detailed skin analysis using just RGB images from mobile devices. The talk will cover our innovative adaptive quality fusion (AQF) metric and methods for estimating key skin properties like melanin and hemoglobin concentrations.
Part 2: Glasgow-Singapore Joint Initiatives: We'll introduce the growing partnership between the University of Glasgow's School of Computing Science and the Singapore Institute of Technology, highlighting our new Glasgow-Singapore Joint PhD Scholarships. These prestigious awards offer doctoral researchers the unique opportunity to spend 18-24 months in Singapore, combining the expertise of both institutions. There are also industrially driven opportunities to co-supervise a student at Singapore. Please, come along if you are interested in engaging with the schemes.
Full Abstract (Part One):
People love to take selfies, and leveraging this trend for skin analysis on mobile devices can democratize access to everyday skincare. This seminar explores the work on hyperspectral reconstruction for skin analysis, combining mobile imaging technology with AI to extract skin spectra information. We begin with the Hyper-Skin dataset, which includes 330 hyperspectral cubes from 51 subjects, spanning visible to near-infrared wavelengths. This dataset facilitates the development of algorithms for consumer applications in cosmetology and skin well-being. We discuss reconstruction algorithms that use deep learning models to map RGB images to hyperspectral images, enabling detailed skin analysis without expensive hyperspectral systems.
To understand the quality of reconstructed images, we introduce adaptive quality fusion (AQF) metric that combines multiple metrics to evaluate the scientific value preserved in the reconstructions. We highlight skin analysis through inverse problem-solving, where an optical-based skin model estimates melanin and hemoglobin concentrations from the reconstructed spectra. This comprehensive approach enhances our understanding of skin characteristics and demonstrates the feasibility of reconstructing hyperspectral image on mobile devices for skin analysis.
Biography:
Pai Chet currently works as an Assistant Professor at Singapore Institute of Technology (SIT). She obtained her Ph.D. from the Hong Kong University of Science and Technology (HKUST). Before joining SIT, she was a Postdoctoral Fellow at the University of Toronto and a Research Associate at the University of Guelph. Her research focuses on applying AI, specifically federated learning on consumer and IoT devices with multimodal IMU and physiological data, and skin spectra analysis with reconstructed hyperspectral images. Dr. Ng's work has been published in prestigious IEEE and ACM journals, including IEEE TMC, IEEE TWC, IEEE JIOT, IEEE JBHI, and ACM TOMM. She has also presented at top conferences such as IEEE ICME, ICC, Globecom, ICASSP, and NeurIPS dataset and benchmark track. She was one of the three recipients for the HKTIIT Post-graduate Excellence Scholarship back in 2019.
Organisation: This event is organised by the Research Student Committee
Grounded radiology report generation with large multimodal models (22 November, 2024)
Speaker: Stephanie Hyland
Abstract:
Machine learning approaches for automated radiology report generation show increasing promise for assisting radiologists in their work. However, for such systems to have clinical impact they must exhibit both strong performance and usability. We demonstrate that performance can be improved by providing models with more realistic reporting context akin to that used by the radiologist, such as the prior study, indication for the study, and lateral view (for chest X-ray reporting). To improve usability, we task the model with generating not only a narrative description of findings, but also localising each finding on the image – a task we call grounded radiology report generation. In this talk, I will describe this novel task, the model we designed to tackle it ("MAIRA-2"), and a new LLM-based evaluation framework ("RadFact") we designed for radiology report generation both with and without grounding.
RadFact here.
Biography: As of 2019, Stephanie is a senior researcher at Microsoft Research Cambridge in the Health Intelligence group. She works on machine learning for healthcare. In 2018, she received a PhD in Computational Biology and Medicine from the Tri-Institutional PhD Program of Cornell University. During her PhD she was situated at the Sloan Kettering Cancer Center in NYC, and later ETH Zürich. Prior to that, she studied theoretical physics at Trinity College Dublin, and applied mathematics (Part III) at the University of Cambridge.
This event is organised by the Biomedical AI and Imaging Lab.
Thumbs Up for Accessibility: Enhancing Non-Verbal Interaction in Technology-Mediated Communication (25 June, 2024)
Speaker: Timothy Neate
Human communication is complex. We do so much more than speak, listen, read, and write. Verbal communication is often complemented by a nuanced range of non-verbal communication, such as body language, gestures, and myriad other means. These broader notions of expression are particularly important for people with communication impairments, as they allow an alternative or complementary means to engage. Despite its clear importance, non-verbal communication takes a minor role in technology-mediated communication. In this talk, I describe our ongoing work, which seeks to respond to this challenge. I detail our investigations into understanding the impact of videoconferencing on communication for people with language impairments and outline challenges and opportunities for supporting diverse communication styles in remote communication. Then, I discuss our ongoing work with discreet and wearable augmented communication devices—detailing how smartwatches, 'earables', smart badges, augmented reality, and other unconventional form-factor devices might support and augment accessible, embodied communication in real-world contexts. Finally, I turn to the future, discuss where I think assistive technologies should progress, and invite your contributions to communication technologies that enable a broader range of expression and inclusion.
Speaker Bio: Timothy Neate is a Lecturer (Assistant Professor in UK) at the Department of Informatics, King’s College London. He is a human-computer interaction and accessibility researcher. His work considers the development of novel interaction techniques and design approaches to make the most of the full range of human capability. He has published work in these areas, mostly focusing on accessible digital content creation/consumption and accessible interaction techniques.
Zoom Meeting ID: 896 4765 1371
Passcode: 727303
Exploring Generative Care Futures with Older Adults (18 June, 2024)
Speaker: Jacob Sheahan
Abstract: The mainstream adoption of generative artificial intelligence (AI) tools has brought many challenges, not least of which has been how we conceive of the future and later life. While efforts to envision and create health technologies with older adults have grown, the adoption of generative systems is now reinforcing many of the stigmas and biases we have long sought to reduce in technology studies. Framing the techno-determinist visions of generative AI as both a feature and tool for critique, I discuss two recent studies examining generative stories and futures of ageing and care with older adults. As we address the challenges of ageing populations and overburdened care systems, can technology designers realise the models of care that really support and enable older adults?
Bio: Jacob Sheahan is a Research Fellow at the University of Edinburgh’s Institute of Design Informatics and Advanced Care Research Centre, where he is currently exploring how to enhance networks of care in later life. With a background in industrial design and a PhD in interaction design from RMIT University, Melbourne, Jacob’s research is interdisciplinary and collaborative, partnering with local communities and organisations to design technologies for socially complex contexts, from ageing to health to safety.
Zoom Meeting ID: 893 6748 4658
Passcode: 520785
Using AI-Enhanced Social Robots to Improve Children's Healthcare Experiences (30 April, 2024)
Speaker: Dr Mary-Ellen Foster
I will describe an ongoing project where we are developing a social robot, based on the Nao platform, to be deployed in two children’s emergency departments to help patients cope with medical procedures that may be painful and distressing. Intravenous Insertion (IVI) was identified as an appropriate procedure: this is one of the most commonly performed procedures in the context of children seeking medical care, and also one that can be painful and distressing for the child and for their parents or caregivers. A social robot was found to be effective in this context; however, the behaviour of that robot was fully scripted, significantly limiting its ability to respond to the child’s state during the course of the procedure. To address the limitations of previous studies, our robot system is designed to use AI planning techniques to allow it to adapt flexibly during an interaction.
In this talk, I will begin by describing how we have engaged with stakeholders throughout the project, including staff, patients, and caregivers at two large Canadian teaching hospitals. I will then present the robot system that we have developed based on those interviews, focus groups, and workshops. The robot system is currently undergoing user testing in the target hospitals, with the goal of a two-site Randomised Clinical Trial to be carried out before the end of 2024.
Zoom Meeting ID: 837 6350 2550
Passcode: 286749
Funding Opportunities for Healthcare Technologies (03 April, 2024)
Speaker: Dr Caroline Hogarth*, Dr Louise Mason**, Dr Hao***
The talk will focus on healthcare technologies funding opportunities both external to and within Glasgow University. It will highlight the dynamic landscape of funding available, including broader translational and commercialisation options like MRC Catalyst Funding, and Innovate UK which supports transformative research endeavours. Additionally, the talk will provide an overview of funding opportunities within the different Impact Accelerator Accounts (IAA) available here at Glasgow. The presentation will include and IAA case study from Dr Hao Gao (Maths and Stats) will illustrate how these funding avenues have driven innovation in healthcare technologies.
Zoom details:
Meeting ID: 890 8494 8981
Passcode: 500251
The RadioMe Project - Supporting People with Dementia through Adaptive Radio (19 March, 2024)
Speaker: Patrizia Di Campi San Vito
The RadioMe project set out to create an adaptive live radio system for people with dementia with reminder capabilities and agitation detection and mitigation with calming music. It is an interdisciplinary project between the University of Plymouth, the Anglia Ruskin University in Cambridge and the University of Glasgow and includes experts in music computation, dementia, music therapy, machine learning and human computer interaction. In this talk we will set out the motivation and goals of the project and discuss the steps towards implementing our current prototype.
Zoom Meeting ID: 810 8234 8522
Passcode: 237685
Journal Club - Shapley Values for Feature Selection: The Good, the Bad, and the Axioms (23 August, 2023)
Speaker: Narinder Kaur - PhD Student
We will be discussing the following paper: 'Shapley Values for Feature Selection: The Good, the Bad, and the Axioms'
Abstract:
The Shapley value has become popular in the Explainable AI (XAI) literature, thanks, to a large extent, to a solid theoretical foundation, including four “favourable and fair” axioms for attribution in transferable utility games. The Shapley value is probably the only solution concept satisfying these axioms. In this paper, we introduce the Shapley value and draw attention to its recent uses as a feature selection tool. We call into question this use of the Shapley value, using simple, abstract “toy” counterexamples to illustrate that the axioms may work against the goals of feature selection. From this, we develop a number of insights that are then investigated in concrete simulation settings, with a variety of Shapley value formulations, including SHapley Additive exPlanations (SHAP) and Shapley Additive Global importancE (SAGE). The aim is not to encourage any use of the Shapley value for feature selection, but we aim to clarify various limitations around their current use in the literature. In so doing, we hope to help demystify certain aspects of the Shapley value axioms that are viewed as “favourable”. In particular, we wish to highlight that the favourability of the axioms depends non-trivially on the way in which the Shapley value is appropriated in the XAI application.
This event is organised by the Healthcare Informatics Lab.
AI in Pervasive Well-Being and Healthy Ageing (29 June, 2023)
Speaker: Workshop
Over the past decade, paradigm shifts have been made towards the way healthcare is delivered and managed. Emerging pervasive sensing technologies, coupled with advanced data analytics, have enabled real-time personalised and environmental monitoring. These technologies have the potential to transform clinical practice in terms of diagnostics, prognosis, preventive healthcare, and rehabilitative/assistive technologies. To enable these systems, we need to understand the challenges in developing AI algorithms to handle heterogeneous, varying quality and imbalanced data. Academics, industry and NHS should work together to develop reliable and trustworthy technologies as well as Deep Learning brain-based algorithms that are able to handle and interpret continuous streams of heterogeneous, multi-modal data.
This workshop aims to bring together academics, industry and NHS related organisations with the goal to highlight opportunities for collaboration. We plan to:
- Promote our technologies and Brain-based AI tools for adoption in the NHS and industry
- Strengthen our current industrial partnerships and seek to establish new ones
- Discuss state-of-the art work in the area of pervasive sensing and healthy brain imaging and how to exploit these to enable innovative solutions
Registration: https://www.eventbrite.co.uk/e/ai-in-pervasive-well-being-and-healthy-ageing-tickets-609375196617
Abstract Submission: https://easychair.org/account/signin_timeout?l=Bkux0ePKTsJx3rMbenFqo2
Medical AI: addressing the validation gap (22 March, 2023)
Speaker: Gael Varoquaux
Abstract:
Machine-learning, which can learn to predict given labeled data, bares many promises for medical applications. And yet, experience shows that predictors that looked promising most often fail to bring the expected medical benefits. One reason is that they are evaluated detached from actual usage and medical outcomes.
And yet, test runing predictive models on actual medical decisions can be costly and dangerous. How do we bridge the gap? By improving machine-learning model evaluation. First, the metrics used to measure prediction error must capture as well as possible the cost-benefit tradeoffs of the final usage. Second, the evaluation procedure must really put models to the test: on a representative data sample, and accounting for uncertainty in model evaluation. I will discuss advanced topic on these questions.
For medical applications, predictions should come with associated confidence. It is important to evaluate these confidence with adequate metrics. Here, the difficulty is to control individual probabilities, as each individual is observed only once. I will explain a procedure to measure how far a predictor is from outputing the ideal individual probabilities, due to intrinsic uncertainty [1].
Predictors can be used to reason about possible interventions: for a given individual, what is the potential outcome of an intervention versus no intervention? However, the corresponding inferences require a particular type of control on the error of the predictors [2].
Last but not least, a numerical experiment to benchmark predictors comes with arbritrary sources of variation. Understanding and accounting for this uncontroled variance is important to make well-grounded decisions on which predictive model to use. This is possible with simple procedures [3].
[1] Beyond calibration: estimating the grouping loss of modern neural networks
Alexandre Perez-Lebel, Marine Le Morvan, Gaël Varoquaux
ICLR 2023 – The Eleventh International Conference on Learning Representations, May 2023, Kigali, Rwanda
https://proceedings.mlsys.org/paper/2021/hash/cfecdb276f634854f3ef915e2e980c31-Abstract.html
Biography:
Gael is a research director at the National Institute for Research in Digital Science and Technology (INRIA) at France. He is also the team leader of Soda - Computational and Mathematical Methods to understand health and society with data (https://team.inria.fr/soda/). His research interests encompasses three areas:
- Machine learning and public health, which involves analytics on health databases for personalized medicine and treatment development, biomedical natural language processing and information extration and causal inference.
- Democratizing machine learning which encompasses machine learning on dirty data Missing data in machine learning, machine-learning model evaluation and learning on relational databases.
- Machine learning for mental health, cognition, and brain activity, which encompasses learning models of brain function and its pathologies from brain imaging, biomarkers of mental traits and disorders which encompasses resting-state and functional connectivity Encoding and decoding models of cognition.
He is also the director of scikit-learn operations at Inria foundation and core contributor of several open source projects in scientific computing with python.
Registration is required: https://uofglasgow.zoom.us/meeting/register/tZwrf-ygqjguE9NlUx9-uLqR0IEutLzPDe0K
Healthcare Seminar: CANCELLED (22 February, 2023)
Speaker: Prof. Crispin Miller
Prof. Crispin Miller is the head of bioinformatics at Cancer Research UK Beatson Insitute. He leads the Computational Biology group, which is focused on using data-driven approaches from machine learning to develop a better understanding of the processes that underpin tumour growth and development.
A major aspect of his work is the use of cancer ‘omics data generated by large-scale tumour sequencing projects. These datasets are large enough to use machine learning algorithms that seek to correlate patterns with phenotype. This is allowing the team to explore aspects of tumour evolution, and to ask how the regulatory systems that control gene expression are perturbed in tumour cells.
His group is particularly interested in the regulatory pathways that act downstream of transcription, including the processes that govern how alternative splicing is coordinated across different pathways. Other projects in the group focus on uncovering novel regulatory sequences within the genome, and in making use of comparative genomics to help interpret the genome rearrangements that occur in tumour cells.
Registration is required: https://uofglasgow.zoom.us/meeting/register/tZUtf-msqjIoEtQhY63wGchI-Vaj42GueFsS
Computationally understanding behavioural atypicality in Autism (18 January, 2023)
Speaker: Dr. Tanaya Guha
Abstract: Individuals with Autism spectrum disorder (ASD) have significantly impaired social communication abilities characterised by atypicality in perceiving and producing non-verbal behavioural cues, such as facial expressions and gaze. Such atypicality has been studied mainly through observations by human experts. However, subtle patterns in the behavioural cues may not be easy to capture by visual inspection alone, which underscores the need for objective data analysis and computational methods. This talk will discuss our work on developing computational methodologies to better understand behavioural phenotyping in ASD, particularly looking at facial expressions and gaze. Our goal is to objectively understand and quantify behavioural atypicality in ASD that can inform diagnosis and intervention.
Bio: Tanaya Guha is a Senior Lecturer in the School of Computing Science, University of Glasgow, and an Honorary Associate Professor in the Department of Computer Science, University of Warwick. Her research focuses on developing machine intelligence capabilities to understand human activities and behaviour combining Machine Learning, Computer Vision, and Signal/Speech Processing. She has published over 60 peer-reviewed articles in leading venues in these areas. She serves in the Editorial Board of Scientific Reports, and in the Organizing/Program Committees of several major conferences such as WACV, ICME, ICMI and Interspeech. More information: https://www.tanayag.com
Registration: This event is hybrid and we encourage to attend in person at 422/423 Sir Alwyn Williams Building, School of Computing Science.
Either way, please register your interest here: https://uofglasgow.zoom.us/meeting/register/tZAscuCgrDgvGNEB9piiUZf_mCbyPsEBu4c2
(copy and paste the link text in the browser does not redirect you correctly)
Cardiac MRI segmentation using MATLAB (07 December, 2022)
Speaker: George Amarantidis Koronaios
Abstract:
Semantic segmentation is a common problem in medical imaging. In this seminar, we will examine how MATLAB Tools (medical imaging toolbox and deep learning toolbox) can streamline this process. We will look into the tools available at your disposal and do a deeper dive into an example of semantic segmentation cardiac MRI data. This example will cover streamlining data labelling, transfer learning, and dealing with label imbalance.
Venue: 422 Sir Alywn Williams Building (Join us in person to discuss internship/job opportunities at Mathworks)
(Hybrid Format- https://uofglasgow.zoom.us/meeting/register/tZAsfumpqjkqHdBuQcvARMF5brkCgoR_cLjx)
Biography:
George Koronaios works with mathworks team to support academics with research and teaching. Recently MathWorks released the Medical Imaging Toolbox to visualise, register, segment and label 2D and 3D medical images. This presentation will provide few examples with a focus on semantic segmentation and labeling. Medical Imaging Toolbox™ provides apps, functions, and workflows for designing and testing diagnostic imaging applications. You can perform 3D rendering and visualization, multimodal registration, and segmentation and labeling of radiology images. The toolbox also lets you train predefined deep learning networks (with Deep Learning Toolbox™).
AI for Precision Histopathology: The Road Ahead (17 November, 2022)
Speaker: Prof. Nasir M. Rajpoot
Abstract:
- Large collections of pathology image data offer a potential goldmine of invaluable information, ripe for deep learning of known and deep mining of novel digital histological biomarkers of cancer diagnosis, prognosis, clinical outcome and response to therapy.
- This talk will cover some of the major challenges faced and opportunities offered by the nascent discipline of computational pathology.
Biography:
Nasir Rajpoot is Professor of Computational Pathology at the University of Warwick and Honorary Scientist at the Department of Pathology, University Hospitals Coventry & Warwickshire (UHCW) NHS Trust. Prior to completing his PhD in Computer Science from Warwick in 2001, he was a Postgraduate Research Fellow in the Applied Math program (partially based at the School of Medicine) at Yale University (USA) during 1998-2000 and a Systems Engineering Fellow at PIEAS (Pakistan) during 1994-1996.
Prof Rajpoot is the founding Director of Tissue Image Analytics (TIA) Centre (previously the TIA lab) at Warwick since 2012 and also co-Director of the recently funded £15m PathLAKE centre of excellence on AI in pathology since Jan 2019. The focus of current research in TIA Centre led by Prof Rajpoot is on AI and machine learning algorithms for the study of histological and multi-omic markers of cancer biology, with applications to early detection of cancer and stratification of cancer patients in terms of recurrence, progression and response to therapy. He has been active in the digital pathology community for almost two decades now and has delivered over 80 invited and keynote talks since 2015 at various national and international events and institutions.
Prof Rajpoot recently served as President of the European Congress on Digital Pathology (ECDP), which took place at Warwick in April 2019. Previously, he served as the General Chair of the UK Medical Image Understanding and Analysis (MIUA) conference in 2010 and as the Technical Chair of the British Machine Vision Conference (BMVC) in 2007. He co-chaired several meetings in the histology image analysis (HIMA) series since 2008 and served as a founding PC member of the SPIE Digital Pathology meeting since 2012. He is a Senior Member of IEEE and member of the Association of the Computing Machinery (ACM), the British Association of Cancer Research (BACR), the European Association of Cancer Research (EACR) and the American Society of Clinical Oncology (ASCO).
Prof Rajpoot was recently awarded the Turing Fellowship by the Alan Turing Institute, the UK's national data science institute.
Machine Learning at NHS National Services Scotland (Business Intelligence) (28 September, 2022)
Speaker: Dr Simon Rogers
NHS NSS is a specialist health board, providing services to the other health boards and across the public sector. Within NSS, the Business Intelligence (and more specifically, the Artificial Intelligence Centre of Excellence) provide assistance, expertise, and a technology platform to support projects with an AI component. In this talk, I will introduce NSS BI (including our Seer platform), and discuss some of the work that we are undertaking, including work on the new version of the SPARRA model (predicting admission / re-admission for individuals in Scotland), work on how to safely export trained models from safe-haven environments, and some ongoing work on fairness / inequalities.
Biography:
Dr Simon Rogers is an AI data scientist at NHS National Services Scotland and Honorary Lecturer in Computer Science at University of Glasgow. His research involves the development of Machine Learning and Statistical techniques to help with the analysis of complex datasets. Among his long publication list he has also published a textbook on 'A First Course in Machine Learning', which is an introduction to modern (fairly probabilistic) Machine Learning.
This is a hybrid seminar: Join us at 423 Sir Alwyn Williams Building, School of Computing Science.
Registration is required: https://uofglasgow.zoom.us/meeting/register/tJUkcOqsqz8vHdboNnP6P-_L3F5na54lHlsx
The promised land of AI for Healthcare and lessons learned wandering the desert (20 July, 2022)
Speaker: Dr. Simone Stumpf
Abstract:
AI is touted as the panacea that will cure all the ills of the current healthcare system. In this talk I will provide an overview of my work in technologies for healthcare, well-being and accessibility that will draw out lessons learned and challenges for designing and developing effective healthcare technologies that use AI.
Biography:
Dr. Simone Stumpf recently joined University of Glasgow, UK, as a Reader in Responsible and Interactive AI. She has a long-standing research focus on user interactions with machine learning systems. Her research includes self-management systems for people living with long-term conditions, developing teachable object recognisers for people who are blind or low vision, and investigating AI fairness. Her work has contributed to shaping the field of Explainable AI (XAI) through the Explanatory Debugging approach for interactive machine learning, providing design principles for enabling better human-computer interaction and investigating the effects of greater transparency. The prime aim of her work is to empower everyone to use AI systems effectively.
Tackling long-tailed category distribution under domain shifts (15 July, 2022)
Speaker: Xiao Guo
Abstract:
In this talk Xiao Gu will talk about his recently ECCV accepted paper on 'Tackling long-tailed category distribution under domain shifts' and the related CVPR 2022 challenge.
Machine learning models fail to perform well on real-world applications when 1) the category distribution P(Y) of the training dataset suffers from long-tailed distribution and 2) the test data is drawn from different conditional distributions P(X|Y). Existing approaches cannot handle the scenario where both issues exist, which however is common for real-world applications. In this study, we took a step forward and looked into the problem of long-tailed classification under domain shifts. By taking both the categorical distribution bias and conditional distribution shifts into account, we designed three novel core functional blocks including Distribution Calibrated Classification Loss, Visual-Semantic Mapping and Semantic-Similarity Guided Augmentation. Furthermore, we adopted a meta-learning framework which integrates the three blocks to improve domain generalization on unseen target domains. Two new datasets were proposed for long-tailed classification under domain shifts, named AWA2-LTS and ImageNet-LTS. We evaluated our method on the two datasets and extensive experimental results demonstrate that our proposed method can achieve superior performance over state-of-the-art long-tailed/domain generalization approaches and the combinations.
Biography:
Xiao is a PhD student at the Hamlyn Centre, Imperial College London, UK. He obtained a BEng degree (Honor Student) in Electronic Engineering from Fudan University in 2018 and MRes degree in Medical Robotics and Image Guided Intervention (Distinction & Dean's Prize) from Imperial College London in 2019. My research interests focus on integrating pervasive sensing and deep learning for healthcare. More details can be found at his website: https://xiaogu.site/
Healthcare Seminar: Dr Xianghua Ding & Dr Marwa Mahmoud (22 June, 2022)
Speaker: Dr Xianghua Ding & Dr Marwa Mahmoud
This is a special hybrid event that hosts Dr Marwa Mahmoud that they are going to talk about their research on 'Advance Technology, Empower People: Exploring Social-Technical Approaches for Everyday Health' and 'Vision-focused multimodal behaviour modelling for mental health applications'
In person location: 422-423 Sir Alwyn Williams Building, School of Computing Science, UoG
Online location: https://uofglasgow.zoom.us/meeting/register/tJUucOCrpjovHdLqvVrzDE4XWTHqH9BtT5uP
Title: Vision-focused multimodal behaviour modelling for mental health applications
Abstract:
There is a growing interest from healthcare organisations, academia and industry on automatic prediction, prevention and intervention of mental health issues, but most of the current work depends on non-visual input, such as wearables and mobile phone data or basic analysis of video focussing on facial expressions analysis only. These models do not capture the full picture and overlook complex non-verbal behaviour analysis, which is the basis of many mental disorder diagnoses. Computer vision techniques have not been fully explored in this domain because of the sensitive nature of the data and limited availability of public datasets for training. Moreover, the high dimensionality of the signals collected from video complicates processing.
In this talk, I will present my work on automatic analysis and detection of body gestures and self-adaptors that are related to psychological distress. I will also discuss multimodal behaviour modelling techniques that I adapted to overcome the challenges of data scarcity and noisy complex signals in mental health datasets. Finally, I will also present some of my recent work on modelling gestures and body expressions in infants shedding light on their relationship with their neurodevelopment assessment.
Biography:
Dr Marwa Mahmoud is a Lecturer in Socially Intelligent Technologies in the School of Computing Science at University of Glasgow, and a Visiting Fellow in the Department of Computer Science and Technology at University of Cambridge, UK. Before joining University of Glasgow, she spent 10 years at University of Cambridge, where she obtained her PhD in 2015, then worked as a postdoc for a year before managing to secure the prestigious King’s College Junior Research Fellowship in 2016, which allowed her to start independent research. Her research interests focus on computer vision for social signal processing and multimodal signal processing, especially within the context of affective computing, behaviour analytics, human behaviour understanding and animal behaviour understanding. She applied her research in the areas of automotive applications, mental healthcare, and animal welfare. She is interested in ‘AI for Social Good’, combining computer vision research with health for human well-being and animal welfare applications. She is an elected Executive Committee (EC) Member of the Association for the Advancement of Affective Computing (AAAC), Network Member of Cambridge Trust & Technology Initiative and a member of Cambridge Neuroscience.
Title: Advance Technology, Empower People: Exploring Social-Technical Approaches for Everyday Health
Abstract:
Today, more and more intelligent healthcare technologies that were only available in medical settings are now easily at our disposal for everyday use. However, technical availability does not mean practical usability. There are still quite some challenges for end users, and lay people in particular, to meaningfully engage with intelligent health technologies and health data to put them into effective use in everyday lives. In this talk, I will share my studies on intelligent health technologies for everyday use, including a mobile application based on face reading technologies for health assessment and lifestyle suggestions, and automatic stress sensing technologies for everyday stress management, and highlight several challenges for intelligent health technologies to be integrated into everyday health practices, e.g. due to the lack of health and technical literacy. I will also share some studies on patient-provider communication platforms, and illustrate how they, by simply making resources more transparent and accessible, enable users to engage in learning, and enact agency and strategies for reliable and cost-effective healthcare. Based on work, I will discuss implications, and how they shape my ongoing work to empower people for effective everyday health management.
Biography:
Dr. Xianghua (Sharon) Ding is a Senior Lecturer in Healthcare Technologies in the School of Computer Science at the University of Glasgow. Before moving to Glasgow, she was an Associate Professor at Fudan University, Shanghai, China. She received her Ph.D. from University of California, Irvine, USA in 2010. Her research falls in the areas of Human Computer Interaction(HCI), Computer Supported Cooperative Work (CSCW), and Ubiquitous Computing (Ubicomp). She is interested in social-technical approaches to empower people to manage their health in daily lives, with particular interest in intelligent health sensing and collaborative technologies for preventive health, health literacy, and mental wellbeing. Her work has been published at flagship venues in HCI such as CHI, CSCW, and Ubicomp, and has received Best Paper (CSCW2015) and Honorable Mention (CHI2020) awards. She has also been serving leadership roles in these venues, including Editor for CSCW2021-2022, Subcommittee Chair for CHI2021’s Health and CHI2019’s Understanding People, and Associate Chair for CHI and CSCW. She also led the publication on a special issue on human-centered cooperative computing as a lead guest editor for CCF’s Transactions on Pervasive Computing and Interaction.
Healthcare Seminar & CIVIS Network: Securing our Identity: from Biometric Anti-Spoofing to DeepFakes Detection (25 May, 2022)
Speaker: Prof. Julian Fierrez
In the last decade we have witnessed extraordinary advances in technologies aimed at managing and securing our identity for online and mobile applications including e-commerce, e-health, e-banking, e-learning, and others. This has been enabled by a rapidly evolving mobile market, with smartphones now having impressive computation capabilities and many audiovisual and biometric-specific sensors capable of acquiring high-quality face images, voice, fingerprints, and other biometric information. This context has nurtured the development of biometric technology that can represent in a very distinctive way our individual identity. These advances in biometric identity have come, at the same time, with growing risks. The information secured by biometric models in our smartphones and other computing platforms are nowadays more valuable than ever, and therefore a growing number of attacks are being conducted seeking big returns by faking our biometric identities. This keynote will summarize the main advances in biometric security conducted in the last decade aimed at evaluating the security of biometric systems against presentation attacks (aka spoofing attacks). Additionally, and as a natural evolution of the mentioned security aspects of biometric identities, we will discuss a topic of growing interest nowadays: facial image manipulation techniques, including DeepFakes, and ways to detect such manipulations. These manipulation techniques, boosted by recent advances in deep learning, can nowadays be used for biometric impersonation in very harmful ways. Both lines of research (biometric anti-spoofing and facial manipulation detection) in a sense have the same purpose: in an interconnected world where we interact more than ever via digital representations of ourselves including in many cases biometric information, there is a growing need for securing our digital identities against a growing army of attackers and attacking methods.
Biography: Julian FIERREZ received the MSc and the PhD degrees in telecommunications engineering from Universidad Politecnica de Madrid, Spain, in 2001 and 2006, respectively. Since 2002 he was affiliated as a PhD candidate with the Universidad Politecnica de Madrid, and since 2004 at Universidad Autonoma de Madrid, where he is currently an Associate Professor since 2010. From 2007 to 2009 he was a visiting researcher at Michigan State University in USA under a Marie Curie fellowship. ELLIS Society.
Prof. Fierrez has received best papers research distinctions, including: EBF European Biometric Industry Award 2006, EURASIP Best PhD Award 2012, Medal in the Young Researcher Awards 2015 by the Spanish Royal Academy of Engineering, and the Miguel Catalan Award to the Best Researcher under 40 in the Community of Madrid in the general area of Science and Technology. In 2017 he has been also awarded the IAPR Young Biometrics Investigator Award, given to a single researcher worldwide every two years under the age of 40, whose research work has had a major impact in biometrics.
Registration is required: https://uofglasgow.zoom.us/meeting/register/tJIpcu2pqDgoEtfbxu-X9VKJ-GMZ-8EXD93x
Subscribe to the computing technologies healthcare seminar emailing list here: https://samoa.dcs.gla.ac.uk/events/series.jsp?series=179
Healthcare Seminar: Can Earables Revolutionise Continuous Vital Sign Monitoring? (27 April, 2022)
Speaker: Prof. Fahim Kawsar
Abstract: Do you know that someone has a heart attack by the time you finish reading this abstract? Indeed, every 40 seconds, a heart attack occurs, and a heart attack fatality occurs about every minute. For long, medical science has established that frequent monitoring of heart rate and blood pressure is the key to mitigating significant risks for stroke, heart failure and coronary artery disease. Current gold-standard vital sign monitoring devices are invasive, cause discomfort and interfere with users' activities. We challenge this status quo and ask - can your next earable be the secret weapon to manage your cardiovascular health? We aren't talking PopSci here but the remarkable capabilities of a sensory earable ushering a new pathway to a healthy heart. However, ensuring the accuracy and robustness of in-ear vital sign measurements is the most complex challenge in this vision. This talk will reflect on the algorithms and their systematic characterisations to address this challenge in continuously measuring the five most critical vital signs in our ear - Heart Rate (and Heart Rate Variability), SPO2, Respiration Rate, Temperature and Blood Pressure.
Biography: Fahim Kawsar leads Pervasive Systems research at Nokia Bell Labs, Cambridge and holds a Mobile Systems Professorship in Computing Science at Glasgow. At his Cambridge lab, he studies forms and intelligence of multi-sensory devices to learn, infer and augment human behaviour in three application areas - Digital Health, Quantified Lifestyle and Smart Built Environment. At Glasgow, he is building up a new group to study system and algorithmic challenges for Mobile Systems. Fahim's research has led to developing multiple artefacts for Nokia (e.g., Consumer Wearables, Sensing-as-a-Service, and Camera Analytics). He has (co-)authored 160+ research papers (Six Best Paper Awards) and granted 40+ patents (Two Top Nokia Innovator Awards). Fahim is a frequent keynote speaker across academic and industrial forums, is an AEIC of IEEE Pervasive Computing, sits at the editorial board of ACM IMWUT, serves (d) as a committee member of leading mobile computing conferences, received multiple million-scale research funds, and has a career accumulation of over €5 Million.
Registration is required: https://uofglasgow.zoom.us/meeting/register/tJEvcOiqrjMrEtRUDgwKSAWB3aTbhFha5G1x
Hybrid Format: Room 422-423 Sir Alwyn Williams Building.
Consider subscribing to our emailing list: https://samoa.dcs.gla.ac.uk/events/series.jsp?series=179
Healthcare Seminar & AthenaSwan Session: Cognitive Vision in Robotic Surgery (16 March, 2022)
Speaker: Dr. Stamatia Giannarou
This is a special session organised on behalf of the Computing Technologies for Healthcare Theme and the Athena Swan. The session includes:
- Research talk and Q/A (60 minutes)
- Discussion on career progression and fellowships (45 minutes)
Registration is required: https://uofglasgow.zoom.us/meeting/register/tJwsduqhrDwiHtdMKCADLEHgdNagRGveehZr
Consider subscribing to our emailing list: https://samoa.dcs.gla.ac.uk/events/series.jsp?series=179
Abstract: With recent advances in medical imaging and surgical robotics, surgical oncology is entering a new era that is set to bring major healthcare and socio-economic benefits. The main goal of surgical oncology is to achieve complete resection of cancerous tissue with minimal iatrogenic injury to surrounding tissue. In practice, this often presents a formidable challenge to surgeons. Surgery on tumours residing within the brain is particularly demanding, and the prognosis for patients afflicted with such tumours remains very poor. Intrinsic brain tumours are highly infiltrative making it difficult to distinguish tumour tissue from surrounding tissue. Moreover, it is imperative to preserve unaffected brain tissue, which is delicate, often eloquent, and has little capacity for regeneration.
The aim of my research is to integrate multimodal intraoperative imaging and navigation technologies into a cognitive robotic platform. In this talk, I will present an intraoperative vision system for surgical navigation and real-time tissue characterisation during robot-assisted neurosurgery to improve both the efficacy and safety of tumour resections. The focus will be on the recovery of 3D morphological structures in the presence of tissue deformation, the efficient robot-assisted tissue scanning with imaging probes and the tissue characterisation for on-line diagnosis support.
Biosketch: Stamatia (Matina) Giannarou received the MEng degree in Electrical and Computer Engineering from Democritus University of Thrace, Greece in 2003, the MSc degree in communications and signal processing and the Ph.D. degree in image processing from the department of Electrical and Electronic Engineering, Imperial College London, UK in 2004 and 2008, respectively. Currently she is a Royal Society University Research Fellow and a Lecturer in Surgical Cancer Technology and Imaging at the Hamlyn Centre for Robotic Surgery, Department of Surgery and Cancer, Imperial College London, UK. Her research focuses on enhanced surgical vision for intraoperative navigation in minimally invasive and robot-assisted operations. In 2017, she won “The President’s Award for Outstanding Early Career Researcher” at Imperial College London. She has been selected as a member of the IdeasLab of Imperial College London on the “Frontiers of Imaging” at the World Economic Forum Annual Meeting of the New Champions 2016 in Tianjin, China. She received best paper awards at international conferences and workshops including the IPCAI 2016, AE-CAI-MICCAI 2020, IPCAI 2020, AE-CAI-MICCAI 2021. She has also been invited to present her work at a number of international workshops and symposia. She is a regular reviewer for high impact journals and conferences in the fields of medical robotics, medical imaging and biomedical engineering and the chair of the annual Hamlyn Winter School on Surgical Imaging and Vision.
From Risky to Trustworthy AI in Healthcare (16 February, 2022)
Speaker: Dr. Karim Lekadir
Abstract: Amid hope and hype, artificial intelligence (AI) is widely regarded as one of the most promising and disruptive technologies for future healthcare. The application of medical AI has the potential to increase the productivity and efficiency of clinicians, improve medical diagnosis and treatment, optimise the allocation of human and technical resources, and lead to better health outcomes for patients and citizens. However, there are currently several technical, clinical, ethical and legal risks associated with medical AI that have limited its deployment in the real world. This talk will discuss these risks, including the potential lack of clinical safety, the limited generalisability of the AI solutions across settings, and important ethical issues such as algorithmic bias against under-represented groups. I will also discuss the need for guidelines and best practices to support the design, development and deployment of future AI tools in healthcare that are accurate and robust, but also trustworthy and ethical, to maximise their acceptance and adoption by medical professionals and patients alike.
Biography: Dr. Karim Lekadir is a Ramon y Cajal Researcher and Director of the Artificial Intelligence in Medicine Lab at the Universitat de Barcelona (BCN-AIM). He holds a PhD from Imperial College London (UK) and was previously a visiting scholar at Stanford University (USA). His current research focuses on the development of data science and machine learning approaches for the analysis of large-scale biomedical data, including imaging, clinical, lifestyle, and mobile data. The software he developed during his PhD for cardiac functional quantification has been CE marked and commercialised by CMRtools, and is now used in more than 250 clinical centres worldwide. He is the Coordinator of the following Horizon 2020 projects: euCanSHare (2018-2022), developing a big data platform for cardiovascular research; EarlyCause (2019-2023), which investigates multi-morbidity using experimental and data science approaches; and EuCanImage (2020-2024), which is building a federated artificial intelligence environment for cancer imaging. He is also work package leader in the longITools H2020 project (2019-2024), developing a mobile app for cardio-metabolic risk prediction based on exposome data. In addition, Karim is General Chair for the MICCAI 2024 Conference (Medical Image Computing and Computer-Assited Intervention) which for the first time will take place in Africa – in Marrakesh, Morocco. He is an Associate Editor of IEEE Transactions on Medical Imaging.
Affective Intelligence and Robotics for Well-being (02 February, 2022)
Speaker: Prof. Hatice Gunes
This is a special session organised on behalf of the Computing Technologies for Healthcare Theme and the Athena Swan. The session includes:
- Research talk and Q/A (60 minutes)
- Discussion on career progression and fellowships (30 minutes)
Registration is required: https://uofglasgow.zoom.us/meeting/register/tJ0od-msqTotHdMlo7hMP2WxCs8jkbNj6J00
Short summary of research talk: Designing artificially intelligent interfaces and robots with socio-emotional skills is a challenging task. Progress in industry and developments in academia provide us a positive outlook, however, the artificial emotional intelligence of the current technology is still limited. In this talk, I will present some of our research explorations in this area with applications to well-being, specifically in virtual reality, in work-like settings, and with/for robotic mental well-being coaching.
Biography: Hatice Gunes is a Professor of Affective Intelligence and Robotics (AFAR) and the Head of the AFAR Lab at the University of Cambridge's Department of Computer Science and Technology. Her expertise is in the areas of affective computing and social signal processing cross-fertilising research in multimodal interaction, computer vision, signal processing, machine learning and social robotics. She has published over 125 papers in these areas (h-index=35, citations > 6,300), with most recent works on lifelong learning for facial expression recognition, fairness and affective robotics; and longitudinal HRI for wellbeing. Some of her research highlights include RSJ/KROS Distinguished Interdisciplinary Research Award Finalist at IEEE RO-MAN’21, Distinguished PC Award at IJCAI’21, Best Paper Award Finalist at IEEE RO-MAN’20, Finalist for the 2018 Frontiers Spotlight Award, Outstanding Paper Award at IEEE FG’11, and Best Demo Award at IEEE ACII’09. Prof Gunes is the former President of the Association for the Advancement of Affective Computing (AAAC), and was the General Co-Chair of ACII’19, and the Program Co-Chair of ACM/IEEE HRI’20 and IEEE FG’17. She was a member of the Human-Robot Interaction Steering Committee (2018-2021) and was the Chair of the Steering Board of IEEE Transactions on Affective Computing (2017-2019). In 2019 she was awarded the prestigious EPSRC Fellowship as a personal grant (2019-2024) to investigate adaptive robotic emotional intelligence for well-being, and was named a Faculty Fellow of the Alan Turing Institute– UK’s national centre for data science and artificial intelligence (2019-2021). Prof Gunes is a Senior Member of the IEEE and a member of the AAAC.
Computer Science career in the NHS: The Scientist Training Programme (STP) (25 January, 2022)
Speaker: Andrew Simpson
Computer Science career in the NHS: The Scientist Training Programme (STP)
Andrew Simpson will join us on Zoom on the 25th of January at 6:30pm to talk about the Scientist Training Programme in the NHS. The STP is a three year fully NHS funded training programme, leading to an Clinical Scientist. During training, the student is paid at NHS Band 6 (at a training Annex). The entry requirements are: An undergraduate degree in either Computer Science, Mathematics or Scientific Engineering.
Computer Scientists who are Clinical Scientists can and do:
- Develop medical software and technology
- Use that software/technology clinically on patients (in theatres, on wards, etc.) (Under Annex A of the Medical Device Regulations)
- Understand and be involved in the research of the science behind the diagnostic test
- Advise doctors on the results and on the technology available for patients.
All as a state registered healthcare professional in a truly unique, in demand and rewarding role.
Higher Specialist Scientific Programme (HSST)
As your career progresses, Clinical Scientists are eligible to further train as Consultant Clinical Scientists in Clinical and Scientific Computing, to demonstrate significant expertise at the intersection of Computer Science and Healthcare.
STP Equivalence
This is portfolio route by the Academy of Healthcare Sciences, where the pre-registrant demonstrates equivalency to the Scientist Training Programme outcomes. A master's degree is not required although the pre-registrant must demonstrate working to master's level.
Route II
This route allows a work-based competency learning route for those who have a masters and relevant experience. The pre-registrant works towards and compiles a portfolio of evidence, demonstrating competency in Clinical Computing to the level of Clinical Scientist.
About Andrew:
He studied BSc & MSc Computer Science, worked in IT industry for a while and he is now training as a clinical scientist in physiological measurement & clinical computing, under Route II, in the James Cook University Hospital's Medical Physics Department.
(For more information email Dr. Tim Storer: timothy.storer@glasgow.ac.uk)
Healthcare Seminar: Towards Bayesian phylogenetics via systematic search and gradient ascent (12 January, 2022)
Speaker: Prof. Frederick Matsen
Phylogenetic (evolutionary tree) inference is a key tool for understanding evolutionary systems. This includes viral adaptation and genomic epidemiology, as well as the antibody response to infection and vaccination. Bayesian phylogenetic analysis allows us to assess and integrate out tree uncertainty to obtain more reliable estimates of other model variables of interest (e.g. transmission rates). However, Bayesian posterior distributions on phylogenetic trees remain difficult to sample despite decades of effort. The complex discrete and continuous model structure of trees means that recent inferential methods developed for Euclidean space are not easily applicable to the phylogenetic case. Thus, we are left with random-walk Markov Chain Monte Carlo (MCMC) with uninformed tree modification proposals; these traverse tree space slowly because phylogenetic posteriors are concentrated on a small fraction of the very many possible trees.
In this talk, I will give a relatively non-technical overview of the work we have done to enable Bayesian phylogenetic inference via optimization. This work has led to a new discrete inferential target, which we call the "subsplit directed acyclic graph," and a new algorithm that will allow us to infer this structure using methods analogous to much faster maximum-likelihood (point-estimate) methods for phylogenetics. I will also describe how, once this structure is in hand, we can perform variational inference for continuous parameters via stochastic gradient descent.
Biography:
Dr. Frederick “Erick” Matsen is an expert in computational biology, which is the science of using biological data to develop computer algorithms, or programs, to understand biological systems and relationships. His research team has developed new methods to analyze data generated by sequencing the DNA of viruses, immune cells and complex environmental samples containing many microorganisms. The team also pursues more abstract questions about the methods used to construct evolutionary trees. Another focus of Dr. Matsen’s work is on improving software used in computational biology, both by developing open source tools and by contributing to work on larger, collaborative projects.
Registration: https://uofglasgow.zoom.us/meeting/register/tJYsf-2tpjkqHte7oAoHA8svaCuDku4j0eJ8
NLP Applications in Mental and Physical Health (01 December, 2021)
Speaker: Prof. Nazli Goharian
Abstract:
With the ever-increasing usage of social media for either explicitly seeking help or for simply sharing thoughts and feelings, we, in the computational disciplines, have the opportunity to utilize such data for building datasets, models, and doing analysis. In the first part of my talk, I will share our collaborative work done at the Information Retrieval Lab at Georgetown University on detecting mental health concerns on social media posts. The first application is on a dedicated mental health forum where the users who register to share and communicate their thoughts and feelings are suffering from some sort of mental distress (sadness, depression, potential of self-harm….). The task is to triage the severity of users’ posts to detect early the potential of self-harm as well as to evaluate the impact of forum activities and conversations on the users during a period of time. In the second type of platform, i.e., non-dedicated, I focus on the question of whether we can detect if a user is suffering from any one or more of the nine mental health conditions, only using the *general language* of the user; that is, the posts are not in mental health [sub]forums nor have any mental health related words. For addressing this question, we had to construct large scale datasets; I will explain how we have identified the diagnosed users, and how carefully selected the controls. Further I will show the results of several baselines to detect the conditions. To conclude this segment of the talk, I will present our preliminary efforts in summarizing mental health posts.
In the second part of the talk, I switch to physical health, and more specifically, to our efforts to address the discrepancies in the radiology reports. Each radiology report is written by residents and reviewed by the attending physician. The question we worked on was how we can detect significant discrepancies in these reports. This system is in use and is made available to the residents in training.
I will conclude with glimpses of additional health related projects of our lab.
Biography
Nazli Goharian is Clinical Professor of Computer Science and Associate Director of the Information Retrieval Lab at Georgetown University, which she co-founded in 2010. She joined the Illinois Institute of Technology (IIT) from industry in 2000. Her research and doctoral student mentorship span the domains of information retrieval, text mining, and natural language processing. Specifically, her interest lies in humane-computing applications such as medical/health domain. Joint with her doctoral students, she received an EMNLP 2017 Best Long Paper Award and COLING 2018 Honorable Mention both for papers on mental health and social media. For contributions to undergraduate and graduate curriculum development and teaching excellence, she was recognized with the IIT Julia Beveridge Award for faculty (university-wide female faculty of the year) in 2009, the College of Science and Letters Dean’s Excellence Award in Teaching in 2005, and in 2002, 2003, and 2007, the Computer Science Department Teacher of the Year Award. She served as Senior/Area Chairs at ACL 2018, ACL 2019, ACL 2020 and ACL 2021. She is co-chair of SIGIR Women in Information retrieval (WIR) since 2019, focusing on gender pay inequity and women leadership.
Registration is required to attend: https://uofglasgow.zoom.us/meeting/register/tJMtdOGtrT4iE9aX2cDxzQ6TbisiGWEn7Y-M
Deep learning for medical image analysis (02 November, 2021)
Speaker: Dr. Alison ONeil
Radiologists are under pressure to handle an ever-increasing volume of medical imaging. In the meantime, deep learning solutions have demonstrated impressive performance for imaging tasks of classification, segmentation and translation, opening up opportunities for AI to assist and automate imaging workflows. Training deep learning solutions for real-world healthcare applications involves ethical, legal and practical performance considerations. As we look to scale deep learning to a wide range of clinical applications, we also need to find ways to reduce reliance on pixel-level expert annotations whilst retaining clinically acceptable accuracy. This talk will cover some of Canon’s research in this area.
Biography:
r Alison Q O’Neil is a Principal Scientist in the AI Research Team at Canon Medical Research Europe and Honorary Research Fellow at the University of Edinburgh. She leads an AI Research team at Canon who focus on imaging and natural language processing for healthcare problems. Her research interests span techniques for learning with less, multimodal learning, knowledge informed machine learning, and causality.
Registration is required to attend the event: https://uofglasgow.zoom.us/meeting/register/tJUuf-2prD0sG91BDJPMlW9HKqBz6itv8CgP
Engaging youth with painful conditions in virtual care: Self-management innovations during and beyond the COVID-19 pandemic (05 October, 2021)
Speaker: Dr. Jennifer Stinson
Dr. Stinson leads the iOUCH lab (improving outcomes in child health using digital health technologies) in The Research Institute at the Hospital for Sick Children in Toronto. Her program of research is focused on improving the way healthcare is delivered to children with life-threatening and chronic illnesses and their families in Canada using the latest in information and communications technologies (ICTs). More specifically, her research focuses on the use of ICTs to (a) assess and manage disease-related pain and other symptoms and (b) deliver innovative disease self-management and transitional care programs to these at-risk populations. During this talk she will describe the user-centred design approach she employs to build virtual care self-management pain solutions, discuss research on the impact of CAVID-19 pandemic on youth with chronic pain in Canada and the development of the Power Over Pain Portal to improve equity and access to pain care in Canada. Finally, she will discuss key lessons learned regarding virtual care for clinical and research.
Lab website - https://lab.research.sickkids.ca/iouch/
Biography:
Dr. Jennifer Stinson is the inaugural Mary Jo Haddad Nursing Chair in Child Health and a Senior Scientist in the Child Health Evaluative Sciences (CHES) research program in the Research Institute at The Hospital for Sick Children (SickKids) in Toronto. She is also an Advanced Practice Nurse in the Chronic Pain Program in the Department of Anesthesia and Pain Medicine at SickKids and a Professor in the Lawrence S. Bloomberg Faculty of Nursing, the Institute of Health Policy, Management and Evaluation and Institute of Medical Science at the University of Toronto.
Registration is required:
HealthCare Seminar: Predicting outcomes after the onset of "psychosis" (02 July, 2021)
Speaker: Dr. Rajeev.Krishnadas
Biography
Dr Rajeev Krishnadas is a visiting consultant at the Priory Hospital Glasgow. He is also a consultant psychiatrist at NHS Greater Glasgow and Clyde and an Honorary Senior Clinical Lecturer at the University of Glasgow. He also sees adults with a wide range of mental health problems, like depression, psychosis, anxiety and bipolar disorder. His particular area of interest is diagnosis and treatment of adults with ADHD.
Dr Krishnadas completed his basic medical training and psychiatric training from Bombay University, India. He then worked as a consultant psychiatrist in India before moving to the UK, bringing extensive experience in managing patients who speak Malayalam, Tamil and Hindi. He then completed his advanced training in general adult psychiatry along with a PhD in psychological medicine, from the University of Glasgow.
To attend you need to register here:
https://uofglasgow.zoom.us/meeting/register/tJMsdO6tpzksHN0ai5MzpOoM6UtEn3ISk3Qr
International Workshop on Artificial Intelligence and Mental Health (08 June, 2021)
Speaker: https://socialcdt.org/aimh/
The World Health Organisation states that mental health problems costs the global economy one trillion US dollars each year, whereas in UK, mental health services report that 19.7% of people over 16 years old show symptoms of anxiety and depression. The latest interactive technologies of social robots and virtual reality, powered by Artificial Intelligence (AI) promise new approaches for clinical treatment of psychiatric, developmental and cognitive problems. This workshop brings together experts in AI, computing and mental health, from both academia and industry, that work towards the development of new, computing based methodologies for detection, treatment and analysis of mental health issues. Besides providing an extensive overview of the state-of-the-art in the domain, the workshop aims at helping young researchers (including PhD students and postdocs) and raise awareness of multidisciplinary opportunities of computing and medical sciences in mental health.
Speakers:
- Dr. Nicholas Cummins
Title: Speech analysis for mental health: opportunities and challenges - Prof. Helen Minnis
Title: Social Signal Processing in Attachment - Prof. Mohamed Chetouani
Title: Putting the social interaction at the center of mental health analysis and modeling with AI-based approaches - Dr. Esther Papies
Title: The role of habits in health behaviour: Challenges and opportunities for digital interventions - Dr Pietro Cipresso
Title: Computational Psychometrics integrating artificial intelligence, virtual reality and mental health
Organised by Computing Technologies for HealthCare and Social AI CDT. For more information and registration details visit the official website.
Computational Biology Conference (27 May, 2021)
Speaker: Prof Robert Insall, Dr Breda Cullen, Dr Richard Reeve, Dr Mayetri Gupta
Organised by staff and PhD students, the First University of Glasgow Computational Biology Conferences aims to bring together researchers across the University of Glasgow who are interested or work in the field of computational biology. Topics of interest including but not limited to: computational approaches in omics, systems biology, population genetics, medical imaging, public health and clinical data. The conference will take place in the afternoons of 27th and 28th of May. We are pleased to confirm our keynote speakers: Prof Robert Insall, Dr Breda Cullen, Dr Richard Reeve, and Dr Mayetri Gupta.
We welcome abstract submissions from early career researchers and PhD students. Abstract deadline is April 30th, 2021. Abstract submission form available on our website: https://cbc.dcs.gla.ac.uk/
Register to attend here.
If you have any questions, please do not hesitate to drop us a message:
HealthCare Seminar: Counting complexity meets digital health (26 May, 2021)
Speaker: Dr Kitty Meeks
Abstract:
Which characteristics should be used to determine whether a patient is offered routine cancer screening? Are there two or three qualitatively different types of heart failure? Which journeys should be forbidden to restrict the spread of an infectious disease?
Data-driven approaches to answering any of these questions - as well as many others in the field of digital health - typically involve searching for a single mathematical object which is optimal with respect to some criterion. For example, we might aim to partition patients into a fixed number of groups or "clusters" in a way that minimises the maximum "difference" in the characteristics of patients assigned to the same cluster.
However, there will often be many solutions that are equally good with respect to our chosen criterion, in which case it is misleading to consider just a single example: if there are many optimal ways to split our patient group into clusters, and there is little agreement between these optimal solutions about which patients belong to the same cluster, then we should not draw conclusions based on just a single optimal solution. It is therefore important to find out more about the whole set of good solutions.
Unfortunately, in most settings, even finding a single optimal solution is a very computationally challenging problem, and finding all good solutions (or even estimating how many of these there are) is even more difficult.
This talk will contain many more questions than answers. In October I will start a 5-year EPSRC fellowship in which I will be developing new theoretical machinery for solving counting, enumeration and sampling problems - with provably efficient and correct algorithms - and exploring the applications of these algorithms to digital health. In this talk I will give a high-level introduction to my proposed methodology, as well as discussing several specific healthcare challenges where I believe this approach can offer new insights. The talk will also act as an open call for collaboration: I would be delighted to hear from others about further potential applications, or opportunities to compare my new approaches to existing techniques.
Biography
As a child, she dreamed of becoming a professional cake decorator. However, it soon became clear that her future was more likely to lie in mathematics. She went on to obtain an MMath in Mathematics and Computer Science at the University of Oxford (Merton College) in 2009; She stayed in Oxford, working under the supervision of Computational Counting. She came to the University of Glasgow in 2014, where she held a lectureship in the School of Mathematics and Statistics for two years. In October 2016 she moved to the School of Computing Science, where she currently hold a five-year Royal Society of Edinburgh Personal Research Fellowship (funded by the Scottish Government).
HealthCare Seminar: Deep Medicine: machine learning meets large-scale epidemiology and population health (28 April, 2021)
Speaker: Prof. Kazem Rahimi / Dr. Mohammad Hossein Mamouei
Abstract: This talk will first provide an overview of the claimed expectations from machine learning and AI in medicine. It criticises the misconceptions around personalised medicine in the context of multi-cause conditions such as cardiovascular diseases. It then provides a general overview of the machine learning research at Deep Medicine with examples of how this is guiding research and could lead to better decision making in clinical practice. Examples will primarily focus on the application of a range of machine learning models to complex Electronic Health Records for risk prediction, co-morbidity and patient clustering, risk factor identification, causal inference and model interpretability.
Kazem Rahimi is a Professor of Cardiovascular Medicine and Population Health, at the University of Oxford and a consultant cardiologist at the Oxford University Hospitals NHS Trust. His research interests include hypertension, heart failure, multimorbidity and cardiovascular risk management, using a variety of methodologies such as individual-patient meta-analysis, large-scale decentralised clinical trials, and digital health technologies.
Kazem leads the Deep Medicine programme at the Nuffield Department of Women’s and Reproductive Health with a major interest in the application of machine learning approaches to electronic health records. He also leadsPEAK-Urban programme.
----
Dr. Mohammadhossein Mamouei is a Machine Learning Scientist at the University of Oxford. As a member of the interdisciplinary research group, Deep Medicine led by Prof Kazem Rahimi, Mo specialises in the applications of machine learning on large-scale electronic health records to extract new insights and develop models for prognostication and diagnostication. He is involved in the PEAK Urban and Informal Cities programmes where he focuses on the effects of environmental and sociodemographic factors on health outcomes.
Before joining the University of Oxford, he was a postdoctoral researcher at City, University of London focusing on the analysis of high-dimensional optical spectra and bio-signals, and a research assistant at University of Southampton focusing on urban mobility.
Mo's educational background is in Applied Mathematics-Systems and Modelling (PhD, City, University of London), and Electrical Engineering (MSc, City, University of London & BSc, Iran University of Science and Technology).
He also leads a team of data scientists at a charity, Apart of Me, that has embarked upon the ambitious project of delivering the first mobile game to help children cope with bereavement.
Healthcare Focused Discussion: Probabilistic Modeling of Postoperative Bleeding Decisions (19 April, 2021)
Speaker: Diana Robinson
Diana Robinson is an incoming PhD candidate in computer science at Cambridge and Student Fellow at the Leverhulme Centre for the Future of Intelligence. Diana specialises in human-computer interaction, philosophy and business. She was a Visiting Scholar at the MIT Media Lab in the Opera of the Future group. Prior to that, she worked as a Commodity Risk Analyst in BP's Integrated Supply and Trading business. She was a Princeton Project 55 Fellow in 2012/13. Diana holds an MBA from the Cambridge Judge Business School and a BA in philosophy from Princeton University.
Focused discussions are events that aim to provide feedback to researchers for work in progress and encourage discussion. Diana's research focus is on representing and modeling uncertainty in decisions around postoperative bleeding following cardiac surgery. Her aim is to see whether a tool that is built on probabilistic programming could be useful in incorporating clinical assumptions, modeling the uncertainty explicitly and reasoning through to likelihood estimates of the next best course of action. One of her interests is in how quantifying uncertainty might impact the social process of decision making, particularly the coordination and handovers between multidisciplinary teams. By developing this from an end user perspective, and co-designing with clinicians, the aim is for clinicians themselves to eventually be able to build and adapt their own models to inform their decisions.
HealthCare Seminar - Precision modelling of brain disease through deep generative modelling (18 March, 2021)
Speaker: Dr. Emma Robinson
Dr Robinson's research focuses on the development of computational methods for brain imaging analysis, and covers a wide range of image processing and machine learning topics. Most notably, her software for cortical surface registration (Multimodal Surface Matching, MSM) has been central to the development of of the Human Connectome Project’s “Multi-modal parcellation of the Human Cortex “ (Glasser et al, Nature 2016), and has featured as a central tenet in the HCP’s paradigm for neuroimage analysis (Glasser et al, Nature NeuroScience 2016). This work has been widely reported in the media including Wired, Scientific American, and Wall Street Journal). Current research interests are focused on the application of advanced machine learning, and particularly Deep Learning to diverse data sets combining multi-modality imaging data with genetic samples. We are particualrly interested in building sensitive models of cognitive development and developmental outcome for prematurely born babies from data collected for the Developing Human Connectome Project (dHCP).
AI for medical imaging applications (04 March, 2021)
Speaker: Matt Muckley, PhD
The event is organised by Dr Sydney N. Williams, Imaging Centre of Excellence (ICE), University of Glasgow
HealthCare Seminar: Trust me, I’m a doctor (25 February, 2021)
Speaker: Prof. John Cleland
Professor John Cleland, Cardiologist & Director of the Robertson Centre for Biostatistics & Clinical Trials
The basis of modern, evidence-based medicine is the randomised controlled trial. This reflects a growing mistrust in the use of observational data to make causal inferences about the effects of lifestyle, diet or medical interventions.
There are many forms of bias in observational data including ascertainment bias, selection bias, information bias, prescribing/intervention bias and confirmation bias. Confounding may or may not be due to one or more of the above.
Amongst these biases, the one that receives the least attention (ie:- usually ignored) in medicine is ascertainment bias, both in terms of ascertaining cases and outcomes. Many analyses depend on medical diagnosis and/or adjudication committees. Although medical opinions may be of value, they are often not based on verifiable facts; a policy of ‘mistrust and verify’ should be applied. Circumstantial evidence is often more compelling than diagnostic opinion.
The application of modern analytical approaches to large datasets is an exciting possibility fraught with hazard. Focussing on associations that create hypotheses and being cautious about any perceived causal relationship is required to avoid damaging academic and clinical reputations and harm to people, patients and populations.
“To err is human, to really foul things up requires a computer.” (attributed to William E. Vaughan, adapted from Agatha Christie, who wrote: ‘To err is human’ but a human error is nothing to what a computer can do if it tries.”)
Biography:
Professor John Cleland is a leading international researcher in heart failure, focusing on improving diagnosis, management and monitoring, and has led large, international clinical trials to study treatments. Professor John Cleland receives substantial funding from the British Heart Foundation to support his research on heart failure. He is a Clarivate Analytics Global Highly Cited Researcher for 2018, one of ten Glasgow researchers recognised as being in the top 1% for citations in their academic field. He also conducted one of the earliest large trials of home telemonitoring for heart failure and continues to promote innovations in this field. His main research interest is heart failure, including its epidemiology and prevention, and development and implementation of guidelines. He has participated in a number of randomised trials to study interventions for heart failure, including the CARE-HF, PEP-CHF and HeartCycle studies. He has been involved in research on the role of myocardial hibernation contributing to heart failure and its treatment (including beta-blockers and revascularisation), diastolic heart failure in the elderly, ventricular resynchronisation, implantable haemodynamic monitoring devices, atrial fibrillation in heart failure and advanced electrophysiology.
Neuroergonomics to Assess and Improve Surgical Performance (11 February, 2021)
Speaker: Dr. Daniel Leff
Neuroergonomics to Assess and Improve Surgical Performance
In this talk, Dr. Daniel Leff will discuss his work within the Hamlyn Centre’s ‘Neuroergonomics and Perception Laboratory’ whose research remit is the evaluation of brain function in surgeons with a view to gaining insights into technical skills training, motor learning, decision-making and fatigue. Recently his focus has been in the detection of changes in brain function that can be used to differentiate high and low demand surgical tasks, facilitate workflow analysis, and which may indicate task induced burden. These factors if reliably detected may form the basis of intelligent feedback loops as means to realise brain computer interfacing to enhance safety.
Biography:
Dr. Daniel Leff is currently a Reader in Surgery working in the Departments of BioSurgery and Surgical Technology, the Hamlyn Centre for Robotic Surgery and the Cancer Research UK Centre at Imperial College London. He is an Honorary Consultant in Oncoplastic Breast Surgery working within the Breast Unit at Imperial College Healthcare NHS Trust. He received his PhD in Surgery from Imperial College London in 2009, working under the supervision of Professor Ara Darzi and Professor Guang-Zhong Yang. Daniel has published over 100 scientific papers in peer-reviewed journals on subjects relating to the application of surgical technologies, assessment of cortical brain function and surgical oncology. His research has been shortlisted for numerous prizes including nominations for the Hounsfield Prize (Imperial College London), Patey Prize (SARS), young scientist award at MICCAI. He has attracted funding from Industry (Hitachi Medical Corp), the Academy of Medical Sciences and Wellcome Trust, and Cancer Research UK.