A RANDOMISED CONTROLLED TRIAL OF A FACILITATED HOME-BASED REHABILITATION INTERVENTION IN PATIENTS WITH HEART FAILURE WITH PRESERVED EJECTION FRACTION AND THEIR CAREGIVERS: THE REACH-HFpEF TRIAL
PUBLIC SUMMARY
OUR AIM:
To find out whether (and how) a home-based rehabilitation programme in people with heart failure with preserved ejection fraction and their caregivers is effective and cost-effective.
WHY THIS RESEARCH IS IMPORTANT:
About half of all people with heart failure have heart failure with preserved ejection fraction (or 'HFpEF'). HFpEF is a complex condition of the heart that affects older individuals who typically have a number of concomitant diseases, including diabetes and high blood pressure. HFpEF has severe impacts on both patients and healthcare systems, including: a markedly reduced ability to undertake activities of daily living, greatly reduced quality of life, and highly increased risk of unplanned hospital admissions, resulting in high NHS costs. Drug and device therapies shown to work in people with the other type of heart failure (heart failure with reduced ejection fraction) do not work in HFpEF. As a result, the 400,000 patients in the UK who have HFpEF are effectively living with untreated heart failure, with potentially devastating consequences for themselves and their families.
With prior National Institute for Health Research (NIHR) funding, we designed a home-based rehabilitation intervention to promote physical and mental wellbeing and support self-management for people with heart failure and their caregivers: 'REACH-HF'. In a randomised pilot study of 50 patients and their caregivers, we showed that people with HFpEF are willing to participate in this type of research and that they engaged well with the REACH-HF intervention.
Recent systematic reviews and meta-analyses support our pilot findings of a potential clinically important effect of exercise-based rehabilitation for HFpEF. However, due to the lack of strong evidence of its effectiveness or cost-effectiveness, cardiac rehabilitation is not routinely recommended for this group of patients. So, this study will undertake a 'definitive trial' to help inform the NHS as to whether REACH-HF should be rolled out to people with HFpEF.
WHAT WE PLAN TO DO:
520 HFpEF patients (and their caregivers) will receive either REACH-HF plus usual care or usual care only. The main patient outcome will be a widely used quality of life measure: the Minnesota Living with Heart Failure Questionnaire. Other outcomes include patients’ mental wellbeing, level of physical activity and hospital admissions, plus caregivers’ quality of life and burden. We will also assess how well the intervention is delivered, what factors may influence responsiveness to the intervention (e.g. patient age, severity of disease, education) and collect information on costs. Interviews with patients and caregivers will help us to inform NHS roll out if the trial is positive.
INVOLVEMENT OF PATIENTS AND CARERS:
Patients and caregivers with lived experience of HFpEF have been involved extensively in the intervention development. A standing Patient and Public Involvement (PPI) group of patients and carers will provide advice during the trial.

Scientific abstract
AIM
To assess the clinical effectiveness and cost-effectiveness of home-based cardiac rehabilitation programme 'REACH-HF' plus usual care (intervention) versus usual care alone (control) in heart failure with preserved ejection fraction (HFpEF) patients and their caregivers.
METHODS
Design:
Multicentre parallel two group randomised (1:1 patient allocation) superiority trial with nested process and health economic evaluations and an internal pilot phase.
Participants:
520 patients with HFpEF and their caregivers.
Setting:
20 sites across England, Scotland and Wales.
Intervention:
REACH-HF is a comprehensive home-based cardiac rehabilitation (CR) and self-management programme informed by evidence, theory, and service users. It comprises the ‘Heart Failure Manual’, a Relaxation CD, a choice of exercise (walking programme or a chair-based exercise DVD), a ‘Progress Tracker’ tool for patients and a ‘Family and Friends Resource’ for caregivers. Participating patients and caregivers work through the manual over a 12-week period with facilitation by a trained healthcare professional (e.g. heart failure specialist nurse, CR nurse or physiotherapist) using both face-to-face and telephone support. Due to the COVID-19 pandemic, we have repurposed the REACH-HF intervention so that (if necessary) it can be delivered entirely remotely through telephone and web-based (where available) contact between healthcare staff and patients/caregivers. A digital version of REACH-HF is currently being developed, and we anticipate that it will be available during the trial.
Control:
Both intervention and control patients will receive usual medical care in accordance with national and local clinical guidelines and a copy of the British Heart Foundation booklet on living with heart failure.
Outcomes:
Primary outcome: Minnesota Living with Heart Failure Questionnaire score at 12-months.
Secondary outcomes: Patient deaths and hospital admissions, blood-borne biomarker, exercise capacity, physical activity levels, psychological wellbeing, generic quality of life, disease-specific quality of life, frailty, and self-management. Caregiver burden, generic quality of life, psychological wellbeing, and self-management. Collected at baseline (pre-randomisation) and 4 and 12 months post-randomisation.
Patients and caregivers will be invited to complete their questionnaire outcomes online (with the option to complete in clinic if not possible). Other outcomes will be collected during a research visit. Subject to ethics/sponsor approval, ‘COVID-19-resilient model’ of data collection is offered to trial centres where clinic visits cannot be undertaken, whether this is at site-level or an individual participant decision - the research team has the ability to collect outcomes via telephone or at home.
Data analysis:
Main analysis will adopt an intention-to-treat approach (based on complete data at 12 months). For continuous outcome measures, we will use mixed-effects regression with a random effect of recruiting site and adjusting for baseline outcome score and minimisation variables. Economic evaluation: Within trial cost-utility analysis over the 12 months. Process evaluation: Case-based mixed methods analysis.
Further details are available in the trial protocol.
PROPOSED TIMETABLE (updated 12th April 2022)
Sept 2021-Mar 2022: Setup (approvals, site selection/recruitment, eCRF/database development):
April 2022-Oct 2023: Screening/recruitment (April 2022-October 2022: 6-month internal pilot)
June 2022-Jan 2024: 4-month follow-up
Jan 2023-Aug 2024: 12-month follow-up
Sept 2024-Jan 2025: Analysis, reporting and dissemination.
Trial Operational Group (TOG)

Professor Rod Taylor. MSc, PhD
Professor of Population Health Research
MRC/CSO Social and Public Health Sciences Unit & Robertson Centre for Biostatistics, Institute of Health and Well Being, University of Glasgow

Professor Chim Lang
Co-Chief Investigator
School of Medicine, University of Dundee

Miss Elizabeth Thomson
Senior Project Manager
Robertson Centre for Biostatistics

Emma Burrell
Project Manager
Robertson Centre for Biostatistics

Anna Placzek
Project Manager
Robertson Centre for Biostatistics

Kate Campbell
Research Administrator
Population Health Facility, University of Glasgow
Project Management Group (PMG)
Professor Colin Greaves – Professor of Psychology Applied to Health President of the UK Society for Behavioural Medicine School of Sport, Exercise & Rehabilitation Sciences, University of Birmingham
Dr Hayes Dalal – Associate Professor, University of Exeter
Professor John Cleland – Director of the Robertson Centre for Biostatistics and Glasgow Clinical Trials Unit (School of Health and Wellbeing), University of Glasgow
Professor Alex McConnachie – Professor of Clinical Trial Biostatistics (Robertson Centre for Biostatistics), University of Glasgow
Professor Emma McIntosh – Professor of Health Economics (Health Economics & Health Technology Assessment), University of Glasgow
Dr Tracy Ibbotson – SPCRN Research Co-ordinator (General Practice & Primary Care), University of Glasgow
Professor Kate Jolly – Professor of Public Health, Applied Health Research, University of Birmingham
Professor Christi Deaton – Professor of Nursing, University of Cambridge School of Clinical Medicine
Professor Mark Petrie – Professor of Cardiology (Institute of Cardiovascular and Medical Sciences), University of Glasgow
Melvin Hillsdon – Associate Professor (Exercise and Health Behaviour), University of Exeter
Professor Patrick Doherty – Professor of Cardiovascular Health and Head of Department, University of York
Dr Julia Frost – Senior Lecturer in Health Services Research (Third Gap Group), University of Exeter
Iain Squire – Professor of Cardiovascular Medicine and University of Leicester & Honorary Consultant Physician (University Hospitals of Leicester), University of Leicester
Valerie Smith – Professor in Midwifery, School of Nursing & Midwifery, Trinity College Dublin
Aynsley Cowie – Consultant physiotherapist in cardiology, BACPR's British Heart Foundation Clinical Research Collaborative research group lead & BACPR Education Lead, NHS Ayrshire & Arran
Claire West – Royal Devon and Exeter NHS Foundation Trust
Louise Taylor – Heart Manual Lead, NHS Lothian
Dr Maureen Travers – Academic Research Co-ordinator, NHS Greater Glasgow and Clyde
Pamela Sandu – Sponsor Research Co-ordinator, NHS Greater Glasgow and Clyde
Nick Hartfield Evans – CEO of Pumping Marvellous Foundation, Pumping Marvellous Foundation

Trial sites
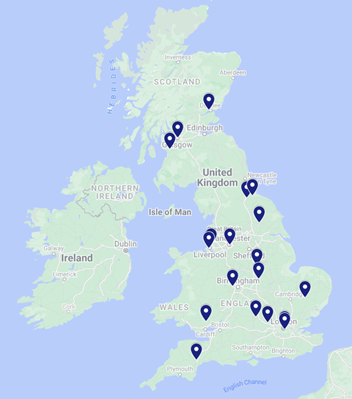
1 Tayside Health Board
2 NHS Ayrshire and Arran
3 NHS Greater Glasgow & Clyde
4 Guy's and St Thomas' NHS Foundation Trust
5 King's College Hospital NHS Foundation Trust
6 County Durham and Darlington NHS Foundation Trust
7 Liverpool University Hospitals NHS Foundation Trust
8 Manchester University NHS Foundation Trust
9 North Tees and Hartlepool Hospitals NHS Foundation Trust
10 West Suffolk NHS Foundation Trust
11 Buckinghamshire Healthcare NHS Trust
12 The Dudley Group NHS Foundation Trust
14 Oxford University Hospitals NHS Foundation Trust
15 Royal Devon and Exeter NHS Foundation Trust
16 York and Scarborough Teaching Hospitals NHS Foundation Trust
17 Wirral Community Health and Care NHS Foundation Trust
18 Leicestershire Partnership NHS Trust
19 Aneurin Bevan University Health Board
20 Cambridge University Hospitals NHS Foundation Trust
21 Royal Free London Hospitals NHS Foundation Trust
|
Site name |
Principal Investigator |
|
Tayside Health Board |
Dr Ify Mordi |
|
NHS Ayrshire and Arran |
Dr Victor Chong |
|
NHS Greater Glasgow & Clyde |
Dr Karen Hogg |
|
Guy's and St Thomas' NHS Foundation Trust |
Dr Andrew D'Silva |
|
King's College Hospital NHS Foundation Trust |
Dr Rosita Zakeri |
|
County Durham and Darlington NHS Foundation Trust |
Prof Jerry Murphy |
|
Liverpool University Hospitals NHS Foundation Trust |
Dr Prathap Kanagala |
|
Manchester University NHS Foundation Trust |
Dr Fozia Ahmed |
|
North Tees and Hartlepool Hospitals NHS Foundation Trust |
Dr Matthew Dewhurst |
|
West Suffolk NHS Foundation Trust |
Dr Justin Zaman |
|
Buckinghamshire Healthcare NHS Trust |
Dr Piers Clifford |
|
The Dudley Group NHS Foundation Trust |
Dr Joe Martins |
|
Nottingham University Hospitals NHS Trust |
Dr John Walsh |
|
Oxford University Hospitals NHS Foundation Trust |
Dr James Gamble |
|
Royal Devon and Exeter NHS Foundation Trust |
Dr Andrew Ludman |
|
York and Scarborough Teaching Hospitals NHS Foundation Trust |
Dr Chris Hayes |
|
Wirral Community Health and Care NHS Foundation Trust |
Dr Joseph Mills |
|
Portsmouth Hospitals University NHS Trust |
Dr Kaushik Guha |
|
Leicestershire Partnership NHS Trust |
Prof Iain Squire |
|
Aneurin Bevan University Health Board |
Dr Philip Campbell |
Patients, caregivers and their families
Patient and Public Involvement Group (PPI)
Trial Steering Committee (TSC) & Data Monitoring Committee (DMC)
Professor Klaus Witte - Chair of Cardiac Device Therapy, Senior Lecturer in Cardiology and Consultant Cardiologist at Leeds Institute of Cardiovascular and Metabolic Medicine University of Leeds and Leeds Teaching Hospitals NHS Trust
Dr Simon Williams (TSC) – Consultant Cardiologist, Wythenshawe Hospital, South Manchester
Professor Susan Dawkes (TSC) – Dean of the School of Health and Social Care/Professor of Nursing and Cardiovascular Health, Edinburgh Napier University
Dr Helen Parsons (TSC) – Associate Professor, University of Warwick
Mr Andrew Leatherland (TSC) – Innovation Programme Manager, British Heart Foundation
Professor Ramon Luengo-Fernandez (TSC) – Associate Professor, University of Oxford
Tom Kennedy (TSC) – Heart Failure Patient Representative
Professor John Norrie (DMC - Chair) – Professor of Medical Statistics and Trial Methodology/Director of Edinburgh Clinical Trials Unit, University of Edinburgh
Professor Abdallah Al-Mohammad (DMC) – Consultant Cardiologist and Honorary Senior Clinical Lecturer, Sheffield Teaching Hospitals NHS Foundation Trust
Professor Ann Dorthe Zwisler (DMC) ann.dorthe.zwisler@regionh.dk MD, cardiologist, Professor in rehabilitation and palliative medicine, University of Copenhagen, Denmark
Contact information
Please contact us at sphsu-reach@glasgow.ac.uk
Conferences and presentations
- Chim Lang. British Society for Heart Failure Investigators Network Virtual Research Meeting - 15th July 2021
- Chim Lang. Cardiac rehabilitation for heart failure, British Cardiovascular Society, June 2023
- Chim Lang. Older people and heart failure: Drugs, devices and exercise. Joint ESC AHA Session. American Heart Association. Philadelphia, November 2023
- Chim Lang. REACH HFpEF trial. British Society for Heart Failure. London, November 2023
- Rod Taylor. REACH HFpEF trial. BSH Research Investigators Network, 6th February, 2024
- Rod Tayor. Exercise based rehabilitation for heart failure patients. Zurich/Londo Heart House, Postgraduate Course of Heart Failure. London. 27th Jan 2024
- Rod Taylor. Exercise-based cardiac rehabilitation and multimorbdity. ESC ACNAP conference, Edinburgh, 24th June 2023
- Rod Taylor. Taking a multimorbidity approach to exercise-based rehabilitation. BACPR Exercise Professionals Group Study Day Programme - 12th May 2023, Birmingham
- Rod Taylor. ’25 years of cardiac rehabilitation research: a look back and look forward’ Heart Rehabilitation in Denmark – What Now? conference. Middelfart, Denmark. 25th April 2023
Study protocol
British Society for Heart Failure Investigators Network Research Meeting




