Nuclear Medicine
Royal Infirmary
As in many places, nuclear medicine at Glasgow Royal Infirmary was first developed by those studying thyroid disorders. Edward M McGirr (later Muirhead Professor of Medicine) –conducted a series of tracer studies in the 1950s and 1960s. He studied the rate of removal of radioactive sodium from muscle and skin in normal and ischaemic limbs, radioactive iodine kinetics in non-endemic goitrous cretinism (with James H Hutchison, later Samson Gemmell Professor of Child Health and radioactive iodine as an aid to the diagnosis of Hashimoto’s Thyroiditis (with I Provan Murray, later Professor of Nuclear Medicine at the University of New South Wales. He also published experience of radioactive iodine treatment of more than 900 patients with thyrotoxicosis.
McGirr was the driving force behind the establishment of the Department of Nuclear Medicine at the Royal Infirmary and its close links with the University Department of Medicine. He was the author in 1975 of an early report on nuclear medicine training in the UK published by the Intercollegiate Standing Committee on Nuclear Medicine. He later served as a member of the National Radiation Protection Board.
John A Thomson, a Glasgow graduate, was appointed to a MacIntyre Research Fellowship in 1959 under Edward McGirr and worked with him in the investigation of radioactive iodine treatment for thyrotoxicosis. He became administrative head of ‘Radioisotopes’ in 1963 on the departure of Murray to Sydney, Australia. Thomson’s interest in the function of thyroid nodules led him to play an important role in the first clinical assessment of an early 7-tube gamma camera. His appointment in 1966 as endocrinologist to the Royal Infirmary permitted Bill Greig to take over what was subsequently known as the Department of Nuclear Medicine.

William (Bill) R Greig, a University of Aberdeen graduate, was appointed as a registrar in the Department of Medicine in 1964, becoming a Wellcome Clinical Research Fellow in 1966 and a senior Wellcome clinical research fellow in 1969. His major research interest was the treatment of thyrotoxicosis by radio-iodine.
In 1969, he proposed the use of iodine-125 instead of the standard treatment with iodine-131.
This was based on the hypothesis that the that the nature of the emissions of 125I meant that it would irradiate the parts of the thyroid cells completing synthesis of hormone to a significantly greater extent than it would irradiate follicular cell nuclei, and thus produce a lower rate of post treatment hypothyroidism than 131I. He conducted a trial of 125I therapy for thyrotoxicosis in more than 350 patients in collaboration with Frank C Gillespie of the Department of Clinical Physics and Bio-engineering and I Ross McDougall (see below). The trial showed that the theoretical advantages of 125I were not translated into better clinical results and that 131I should remain the radio-isotope treatment of choice for thyrotoxicosis.
This was the period of the emergence of technetium-99m labelled radiopharmaceuticals and Greig ensured that his department, which included Lesley Hooper as clinical physicist, was involved in their evaluation, particularly in the case of bone scanning agents as discussed below. Greig retired on health grounds in 1979 and died in 1983 at the age of 47.
I Ross McDougall, a Glasgow graduate, was appointed as a lecturer in Medicine in 1970.
He worked closely with Greig and gained his PhD on clinical and radiobiological studies of 125I in thyrotoxicosis. He spent 1972–74 as a Harkness Fellow with Joseph Kriss at the Nuclear Medicine Department at Stanford University. McDougall took up his Lecturer post again after this fellowship, but returned to Stanford in 1976 as Associate Professor of Radiology and subsequently Professor of Medicine and Radiology.
Denis L Citrin, a Glasgow graduate, was appointed as an SHO in the University Department of Medicine in 1971. He studied bone scanning with 99mTcphosphates in breast cancer as the subject of his PhD, working with Greig and Leslie H Blumgart (St Mungo Professor of Surgery). The series of publications arising from his work were pivotal in establishing the role of isotope bone scanning in the diagnoses and management of bone metastases. Citrin demonstrated the greater sensitivity of isotope bone scanning in diagnosing occult bone metastases in breast cancer patients, but also its limited specificity. His study was one of the first to show the prognostic significance of an abnormal bone scan in this setting. He also published the first comprehensive atlas of bone scanning (with James H McKillop – see below).
On completion of his PhD, Citrin was awarded a Medical Research Council fellowship in cancer medicine at the University of Wisconsin-Madison where he completed a fellowship in human oncology. He remained in the USA practising as an oncologist.
Henry (Harry) W Gray, a Glasgow graduate, was appointed Hall Fellow in 1968 and as a Lecturer in Medicine in 1969. He spent 18 months as a Trainee and Research Fellow at the Nuclear Medicine Department of The Johns Hopkins Hospital in Baltimore working with Henry Wagner on the behaviour of white cells with a view to infection imaging. After his return, and further training in Endocrinology and Diabetes, he was appointed a consultant physician in the University Medical Unit with a special interest in Nuclear Medicine. He was the consultant physician in charge of the Nuclear Medicine department at GRI from 1977 till 2007 with Dr Rodney Bessent, consultant physicist (see below) and latterly with Dr Alison Bolster.

Gray developed a research interest in the clinical aspects of ventilation perfusion (V/Q) lung scanning for pulmonary embolism, and published extensively on its diagnostic accuracy, the use of Bayesian analysis and the clinical implications of findings from V/Q scanning. He also examined the language of V/Q scan reporting and how this language was understood (or not!) by the referring clinicians. In 1996, he was the local Congress President of the European Association of Nuclear Medicine meeting in Glasgow.
Later in his career, Gray studied the efficacy of radionuclide sentinel node imaging in cancer. Working with the head and neck surgeons from Canniesburn Hospital and the Royal Infirmary, this technique was applied to the preoperative investigation of patients with head and neck cancer and melanoma and showed its efficacy. With the surgical lead, he participated in a multicentre European trial on the subject and contributed to international guidelines arising from the trial. Gray retired in 2007.
Ignac Fogelman, a Glasgow graduate, joined the University Medical Unit in 1975 and developed an interest in bone scanning and bone metabolism working with Dr IT Boyle and Rodney G Bessent (see below). From 1977 onwards, Fogelman published a series of articles on the bone scan in metabolic bone disease, categorising for the first time the scintigraphic appearances in this group of conditions. These studies remain the classical and still accepted description of the bone scan appearances of this group of diseases. He also studied the use of whole body retention of radiolabelled phosphonates (using either a whole body monitor or a non-collimated gamma camera) as a quantitative measure of skeletal metabolism and demonstrated the value of this technique in monitoring the progression of metabolic bone diseases and response to therapies.
He was aided by M Linda Smith, later Senior Registrar in the Department, then consultant in nuclear medicine at the Royal Liverpool Hospital. On completion of his training as a Senior Registrar, Fogelman was appointed as Consultant in Nuclear Medicine at Guy’s hospital in 1983 where he continued his work on bone diseases, particularly osteoporosis, and bone scanning for the rest of his career. He published extensively, including several highly regarded atlases of scintigraphic appearances. Fogelman was promoted to Professor of Nuclear Medicine at Guy’s in 1996. He won many awards including the prestigious Sir Godfrey Hounsfield Memorial Award from the British Institute of Radiology (BIR).
He retired in 2015 and died in 2016. In an obituary written by European colleagues he was described as “the father of radionuclide bone imaging”.
James (Jim) H McKillop, a Glasgow graduate, joined the University Department of Medicine as Hall Fellow in 1973, becoming a Lecturer in 1975, Senior Lecturer in 1982 and Muirhead Professor in 1989. Myocardial perfusion imaging using thallium-201 (201Tl) was the subject of his PhD thesis. Working with Rodney Bessent and A Ross Lorimer, he demonstrated its diagnostic accuracy in coronary artery disease and devised one of the first approaches to quantitative analysis of the images. During a two year Harkness Fellowship in Nuclear Medicine at Stanford, he worked with Ross McDougall, Joseph Kriss and Michael Goris on various aspects of nuclear cardiology, bone scanning and infection imaging.
On his return to Glasgow, McKillop continued to work in nuclear cardiology in collaboration with Ross Lorimer, Ian Hutton, Ann Tweddel (all Medical Cardiology) and William Martin (DCPB) resulting in a series of publications. Together they investigated perfusion imaging in the diagnosis of coronary artery disease, its monitoring and its response to treatment. They also investigated its use in hypertensive patients with left ventricular hypertrophy and demonstrated that this group of patients had focal abnormalities of perfusion even in the absence of clinically significant coronary artery disease.
McKillop later developed an interest in tumour imaging. He investigated the efficacy of 201Tl as a tumour imaging agent in a range of cancers. He worked with Colin S McArdle and Timothy G Cooke on the imaging and evaluation of hepatic metastases from colorectal cancer and their treatment using radiolabelled microspheres. McKillop was chair of the Intercollegiate Standing Committee on Nuclear Medicine and of the Administration of Radioactive Substances Committee (ARSAC) of the Department of Health and a Congress President of the European Association of Nuclear Medicine.

Rodney G Bessent, an Oxford DPhil, joined the Nuclear Medicine Department at GRI in 1972 and remained there until his retiral in 2003. Bessent provided the physics support for most of the research studies carried out by the department during that period. His expertise, scientific rigour and constructive criticism were a crucial component of these studies. He was a member of the University Department of Clinical Physics and Bio-Engineering (DCPB). Bessent’s main interest was in developing computing in the Nuclear Medicine Department. He wrote most of the software for the Department’s first gamma camera image processing computer and guided the development through several generations of hardware and software, with the essential input of a succession of assistant medical physicists, to a fully networked departmental image acquisition and reporting system.
His particular interest was in image enhancement and in extracting quantitative information from nuclear medicine images, especially dynamic sequences.
J Brian Neilly joined the Department as a senior registrar in 1990 and was appointed consultant in medicine and nuclear medicine in 1995. He worked with Gray on V/Q imaging and was a co-author of European guidelines on its clinical use. He has a strong interest in postgraduate nuclear medicine education and training. He succeeded Gray as head of the department of nuclear medicine in 2007.
John Davidson (later consultant in Medicine and Nuclear Medicine at Ninewells Hospital) was a Senior Registrar in the Department in the late 1990s.
Fat-Wui Poon, a graduate of Aberdeen, was appointed as Consultant radiologist with interest in Nuclear Medicine at GRI in 1990. His early work was in the early diagnosis and staging of colorectal cancer with Magnetic Resonance imaging in particular. Later on, he became the clinical director of the Positron Emission Scanning (PET-CT) Centre from 2007 to 2012, and worked on the roles of 18F-FDG PET-CT in multiple areas of oncology. Poon was the research lead at the PET Centre between 2012 and 2014.
Sai Han, a graduate of University of Medicine (1), Myanmar, was appointed specialist registrar in Medicine and Nuclear Medicine in 2002 and consultant in Medicine and Nuclear Medicine, GRI and West of Scotland PET-CT Centre since 2007. His MSc from Kings College, London in 2004 was on amyloid imaging. Since 2007, his work has majored upon PET-CT in oncology and has included a time as clinical lead of the PET-CT Centre (2012 – 2016).
Four of the Presidents in the 50 year history of the British Nuclear Medicine Society came from Glasgow Royal Infirmary:
Edward McGirr 1969-70
Jim McKillop 1990-92
Harry Gray 1996-98
Brian Neilly 2012-14
No other hospital has provided as many presidents of this national society.
Professor James H McKillop
Western Infirmary
In the Western Infirmary, the practice of nuclear medicine had its origins in non-imaging studies carried out in the Professorial Medical Unit in the Gardiner Institute. Radionuclide imaging was introduced later by the NHS as an adjunct to its Department of Radiology, principally under Dr Fred Adams, and there was no identifiable department of nuclear medicine.
In 1954, Sir Edward Wayne was appointed Regius Professor of the Practice of Medicine. His special interest in his previous post in Sheffield had been the thyroid gland and this led to the introduction of radioiodine for both diagnosis and therapy in the Gardiner Institute (GI). Much of the work was carried out in collaboration with physicists from the Department of Clinical Physics and Bioengineering (DCPB), in particular Dr James Shimmins and his team, who studied the kinetics of thyroid uptake of radioiodine and began investigating the use of technetium-99m in thyroid studies when it became available in the mid 1960’s. Wayne retired in 1967.
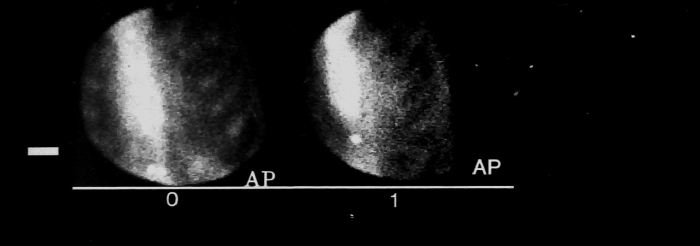
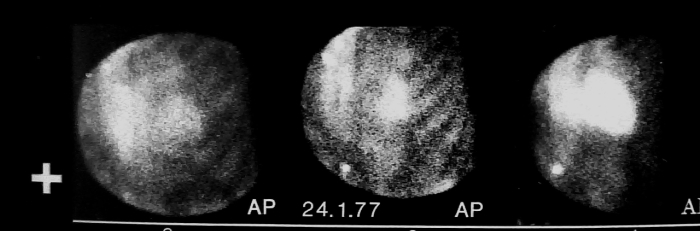
Initially, DCPB provided scientific input from the central department in West Graham Street but senior staff were later based in the Western Infirmary, having offices in the Gardiner Institute.
Patrick (Pat) Horton graduated from Imperial College, London and joined DCPB in 1970. He left in 1979 to take up a post in Riyadh.
Thomas (Tom) Hilditch was a double Glasgow graduate in physics (BSc 1963, PhD 1978) and joined DCPB in 1964. He provided the scientific support underpinning the great majority of the work carried out in the Gardiner Institute from then until his retirement in 2003. Initially based in the central department, he transferred full-time to the Western Infirmary in 1974. In addition, he published extensively in the radionuclide imaging and radiopharmacy literature.
Donald Alexander built up the GI work throughout the 1960s and 1970s with scientific support principally from Dr Patrick Horton and Dr Tom Hilditch; they continued to widen the clinical application of thyroidal uptake and clearance of intravenous radioiodine (iodine-131 and the short-lived iodine-132) and extended the use of technetium-99m. They applied compartmental modelling of kinetic uptake data to obtain estimates of unidirectional clearance and intra-thyroidal binding rates of iodine, making use of a radionuclide scanner to measure thyroid uptake which reduced uptake errors caused by extrathyroidal activity in the field of view of a simple collimated detector. Serial measurements of thyroid uptake became less laborious and more accurate with the introduction of the gamma camera and the ready availability of iodine-123.
Alexander also developed, in collaboration with Keith Boddy, a means of quantifying intrathyroidal iodine at the Scottish Universities Research and Reactor Centre (SURRC) in East Kilbride. Patients were sent to SURRC, where thyroid irradiation was carried out using a neutron beam from the reactor to activate iodine-128 for measurement of the iodine content of the gland.
Wayne was succeeded in 1967 by Graham Wilson, who was also keen to pursue radioisotope studies. He obtained funding for a Bone Metabolism Unit, which opened in 1970, and expanded the collaboration with Keith Boddy at SURRC to include neutron activation analysis. He died in post in 1977.
Deryck Smith was appointed director of the Bone Metabolism Unit and used radioisotopes to measure exchangeable calcium. He also collaborated with Keith Boddy in utilising an in vivo whole body neutron activation analysis system at SURRC for the measurement of whole body calcium. In the late 1970s and early 1980s, he worked with DCPB to develop a novel radioisotope quantitative CT scanner for the measurement of cortical and trabecular bone mineral density. This was used primarily in the investigation of osteoporosis.
The establishment of the MRC Blood Pressure Unit led to the introduction of isotope studies of body electrolytes, largely under the clinical supervision of Dai Davies. He too collaborated with SURRC, initially making use of their mobile whole body monitor to measure naturally-occurring potassium-40. An in-house whole body monitor was built in the 1970s which permitted an expansion in the range of studies; as well as potassium-40 measurements, much work was carried out on exchangeable sodium and potassium using sodium-24 and potassium-43 and on the biokinetics of trace elements such as manganese.
Sir Abraham Goldberg succeeded to the Regius Chair in 1977 and continued the tradition of supporting radionuclide investigations, having himself made important studies on blood diseases using radioiron and radiochromium. This haematology interest was integrated with that already being pursued in the GI by John Dagg.
Alex Elliott, a Stirling graduate in theoretical physics, gained his PhD in in vivo whole body neutron activation analysis from Glasgow in 1974 under the joint supervision of Keith Boddy and Graham Wilson and his DSc in nuclear medicine from Glasgow in 1989. He joined DCPB at the Western Infirmary in 1981, becoming head of department and Professor of Clinical Physics in 1990, and continued to work in nuclear medicine at the Western Infirmary until his retirement in 2009. He was a member of ARSAC and of the Committee on Medical Aspects of Radiation in the Environment (COMARE), chairing the committee between 2005-2015. His major interests were in nuclear cardiology and radiopharmacy.
Henry Dargie, a Glasgow graduate, was a registrar in the renal unit at GRI who then moved to Hammersmith Hospital as senor registrar in cardiology. He was appointed as consultant cardiologist at the Western Infirmary in 1979. In collaboration with Alex Elliott, he developed nuclear cardiology throughout the 1980s and 90s. They used a multicrystal gamma camera in conjunction with novel radiopharmaceuticals such as gold-195m (half-life 30 seconds) to improve the early diagnosis of coronary artery disease, together with investigating the effects of pharmaceutical treatment. A mobile gamma camera permitted studies in the coronary care unit and outside the hospital. They introduced SPECT studies for myocardial perfusion.
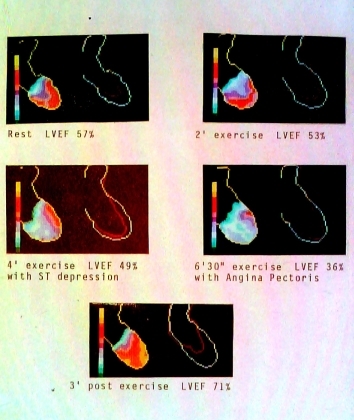
In addition to many scientific papers, several MD theses resulted. Dargie was awarded a personal chair in 1994 (see Cardiovascualar Disease).
Between 1989 and 2009, the Regius Chair was held by John Reid. He had been involved in radionuclide studies in his previous post at Stobhill Hospital and oversaw an amalgamation of this work and that being undertaken at the Western. Ken McColl developed an interest in radioisotopic breath tests, particularly carbon-14 urea for helicobacter and this was a major area of research in the 1990s (see Gastroenterology).
There had been a centralised facility for the preparation of radiopharmaceuticals at the Western Infirmary for several years, but a total replacement was deemed necessary by the Medicines Inspectorate in 1985.
Alex Elliott, in conjunction with Tom Hilditch and Tom Murray (radiopharmacist), obtained NHS funding and designed a new state-of-the-art radiopharmacy, which opened in 1989 and was the first of its kind.
This had the capability to synthesise novel in-house materials to the highest commercial standards and led to several clinical research projects at both the Royal and Western Infirmaries and the Southern General Hospital.
Through the 1990s, Elliott collaborated with the vascular surgeon Alan Mackay to develop a novel radionuclide method to monitor intra-operative leakage of chemotherapeutic agents into the central circulation during isolated limb perfusion procedures for therapy of malignant melanoma.
A Scottish committee was set up in 2002 to investigate the implementation of positron emission tomography (PET), Glasgow being represented by Alex Elliott. With support from the six West of Scotland Health Boards in place at that time, NHS funding was made available for the purchase of a scanner and a cyclotron. Elliott and Tom Murray designed a new facility (including provision for a second scanner) as an extension to the Tom Wheldon Building at Gartnavel General Hospital; the scanner became operational in November 2007. The cyclotron was commissioned in 2008/9, having the capability to produce Fluorine-18, Carbon-11, Nitrogen-13 and Oxygen-15 and was fitted with automated synthesis equipment in a sterile suite. A sterile radiopharmaceutical research laboratory was incorporated also, with much of its equipment provided through the University.
Professor Alex Elliott
Images provided by Professor Alex Elliot



