Obstetrics and Gynaecology
Obstetrics and Gynaecology, the specialities of childbirth and the female reproductive system, were early medical and surgical specialties.
Obstetric Hospitals in Scotland
The Regius Chair of Obstetrics and Gynaecology in Glasgow University was founded in 1815 (see below). 
Its first occupant, James Towers (1757-1820) attempted to found a Glasgow Lying-in Hospital for women in childbirth, as did his son John (1791-1833) who succeeded his father in the chair – a common event for 19th century Scottish clinical chairs! The Glasgow Lying-in Hospital started in 1834, and after The Glasgow Lying-in Hospital started in 1834, and after occupying a number of locations it became firmly established on Rottenrow (rue de roi: the way of the king) in 1880, on the corner of North Portland Street.
Renamed the Glasgow Royal Maternity Hospital and Women’s Hospital, it was expanded to the west as a handsome building with an elegant portico in 1908. Because of the requirement to demonstrate that it was debt free, attempts to obtain a Royal Charter were not successful until 1914.

(There was some resentment that the Royal Samaritan Hospital, essentially a gynaecological facility, had been granted theirs in 1907).
It relocated to the nearby Royal Infirmary as the Princess Royal Maternity Unit in 2001.
Among the distinguished obstetricians at Glasgow Royal Maternity Hospital were Murdoch Cameron (1845-1930), who published a world renowned series of classical Caesarian sections in 1888; and Munro Kerr (1868-1960), who was the dominant figure in British obstetrics in the first half of the 20th century. He was the father of obstetric audit, including the collection of maternal and perinatal morbidity and mortality data.
At the start of the National Health Service in 1948, its most famous NHS consultant was Sir Hector Ross MacLennan (1905-1978. He trained many Scottish consultants; was President of the Royal College of Obstetricians and Gynaecologists (1963-1966); and was knighted in 1965. Subsequent important NHS consultant contributors included Robin Murdoch, Matthew Garrey, Bill Black (who represented Scotland at rugby) and Helen McEwan.
The Queen Mother’s Hospital, linked to the new Royal Hospital for Sick Children at Yorkhill, was opened in 1964. At this time it was the most modern maternity hospital in Europe. Important NHS consultant contributors included Iain McBride (“the Master” in the view of his trainees), James Willocks (unsung, as effectively the first to apply ultrasound in obstetrics while Ian Donald (see below) felt its greater potential lay in gynaecology), Wallace Barr, Alastair Miller and Rob Chatfield.
The Queen Mother’s Hospital closed in 2010 with the opening of the new maternity unit at the Queen Elizabeth Hospital in Govan, and subsequently linked to the new Royal Hospital for Children opened in 2015.
Important NHS consultant contributors at other units included
- Stobhill Hospital, the David Mackay Harts (father and son)
- Southern General Hospital, Arthur Sutherland, James McGarry and Matt Carty
- Lanarkshire, Robert Tennant and Malcolm Black (a major contributor in Rhesus disease – see below, Charles Whitfield)
One of the proudest claims of Glasgow obstetrics and gynaecology is the impact it has had beyond the West of Scotland.
The catalogue of Glasgow trained clinicians and academics who have dominated the specialty in these islands and beyond include Professors Sir Dugald Baird (Aberdeen, a champion of social obstetrics and family planning, alongside Ian Donald (see below).
The other giant of mid-20th century British obstetrics (albeit their views on therapeutic abortion could not have been more different), and Baird’s successor was Iain McGillvray.
Other Professors include
- James Walker (senior) and Peter Howie (Dundee)
- Andrew Calder and Jane Norman (Edinburgh)
- Hugh McLaren, Henry Kitchener and Martin Whittle (Birmingham),
- Gordon Stirrant (Bristol)
- Charles Douglas and Gordon Smith (Cambridge)
- John Bonnar (Dublin)
- Stuart Campbell (Kings College London)
- James Scott and James Walker junior (Leeds)
- John Mcvicar (foundation chair in Leicester)
- James Neilson (Liverpool)
- Hugh Robinson (Melbourne)
- Donald Gebbie (foundation chair in Nairobi)
- Jake Russell (Newcastle), and David Barlow (Oxford).
Many more make up a vast catalogue of prominent NHS consultants across the land.
One of the proudest claims of Glasgow obstetrics and gynaecology - is the impact it has had beyond the West of Scotland
Muirhead Chair of Obstetrics and Gynaecology
This chair was founded in 1911, endowed by the Trustees of Henry Muirhead (1814-1890), and based at Glasgow Royal Infirmary and the Royal Maternity Hospital. As with the Muirhead chairs of Medicine and Surgery, the trustees gave these chairs to the Royal Infirmary rather than the Western Infirmary, because at that time the Western Infirmary did not admit women to medical posts.
- Dr David Fyfe Anderson (1904-1988) was Professor from 1946-1970. He contributed an oral history in an interview with Dr Peter Mackenzie, available at RCPSG and Mitchell library.
His compiled papers are kept in the NHS Greater Glasgow and Clyde Archives.

- Sir Malcolm Campbell Macnaughton (1925-2016), popularly known as “Calum”, was Professor from 1970-1990. Macnaughton embraced the belief that women should not find themselves prisoners of their own fertility, and supported the provision in the National Health Service of contraception, sterilisation and abortion in the West of Scotland. He also advocated the cause of women who were infertile, and was involved in the early clinical trials of Human Menopausal Gonadotrophins for the treatment of anovulation. He was an early advocate of laparoscopy, helping to introduce this technique to gynaecological practice in Scotland.
He played a key role (as the only clinician on its committee) in the development of the 1984 Warnock Report on Human Fertilisation and Embryology. The report became the basis for British legislation on in-vitro fertilisation and embryo research in 1990. He was elected President of the College of Obstetricians and Gynaecologists (1984-1987); elected President of the British Fertility Society (1992-1995); and was knighted in 1986. - Dr Ian Greer was Muirhead Professor from 1990-2001; then Regius Professor from 2001-2006. He merged the separate departments at Glasgow Royal Infirmary / Royal Maternity Hospital and the Queen Mother’s Hospital. He published on the risks of venous thromboembolism in pregnancy, including in women with thrombophilias (genetic or acquired increased activation of blood coagulation). He also researched the pathophysiology of pre-eclampsia (increased blood pressure during pregnancy), showed for the first time that neutrophil activation and an inflammatory response was a feature of the pathophysiology, and also studied its long-term sequelae of insulin resistance, microvascular dysfunction and increased cardiovascular risk. In 2006, he was appointed Dean of the Hull York Medical School before moving to the University of Liverpool as Pro Vice Chancellor, the University of Manchester as Vice President and Dean, then the University of Belfast as Vice Chancellor.
- Dr Scott Nelson was appointed Muirhead Professor in 2008. His research focuses on infertility and pregnancy, reflecting his clinical work leading the largest In Vitro Fertilisation (IVF) unit in Scotland. He is interested in new techniques and “omics”. Currently he is studying factors influencing the outcome of pregnancy and in vitro fertilisation using epidemiological studies and collecting samples for genomics, proteomics and metabolomics. This may allow new treatments and encourage personalised medicine.
Regius Chair of Obstetrics and Gynaecology
This Chair was founded in 1815 by King George III, initially as the Chair of Midwifery, the name being changed by amendment in 1992 at the instigation of Ian Greer. When the Western Infirmary was built, it was based there, and subsequently at the Queen Mother’s Hospital after it opened in 1964.
- Dr Robert Aim Lennie (1889-1961) was Professor from 1946-1954. He had a distinguished military record in both world wars; and a conservative attitude to management of pregnancy complications. He was a man of conservative judgement, and disapproved of surgeons who were too quick to proceed to induction or Caesarian section.
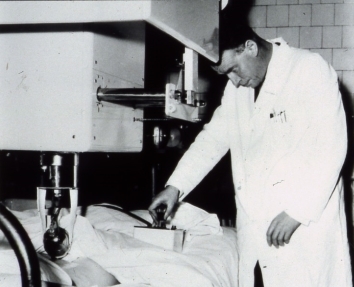
- Dr Ian Donald (1910-1987) was Professor from 1954-1976. He became interested during the Second World War in the possibilities of adapting radar and sonar technology for medical diagnosis. He worked in Glasgow with T G Brown of the scientific instrument makers Kelvin and Hughes to create the first diagnostic ultrasound machine, which allowed visualisation of the fetus in ute

- In 1958, with Brown and John MacVicar, he published their findings in The Lancet. From this pioneering start, ultrasound became an important part of routine monitoring of pregnancy in developed countries worldwide. Donald also pioneered laparoscopy in Scotland; and was involved in the planning and design of the Queen Mother’s Maternity Hospital in Glasgow, which opened adjacent to the Royal Hospital for Sick Children at Yorkhill in 1964.
He was appointed CBE in 1973. A detailed memoir of Ian Donald, written by his obstetrician colleagues James Willocks and Wallace Barr, was published in 2004 by the RCOG Press.
- Dr Charles Whitfield (1927-2018) was Regius Professor from 1976-1992. He was a pioneer in the specialty of maternal and fetal medicine in the UK; and in the assessment and treatment of rhesus disease (haemolytic disease of the newborn) – a major killer of newborn babies in the 1970s. Rhesus disease occurs when a women with rhesus negative blood group is exposed to rhesus positive blood, either during a pregnancy or a blood transfusion. Her body reacts by producing antibodies to destroy these “foreign” blood cells. If she subsequently becomes pregnant, these antibodies can cross the placenta and attack the foetus’s blood cells, causing anaemia and jaundice. Untreated, it can cause stillbirth, learning difficulty, deafness and blindness. Whitfield introduced blood transfusion to the fetus in the womb to give the baby a better chance of survival. Today rhesus disease is uncommon, following the introduction of immunoglobulin injection for exposed women from 1967; however intrauterine blood transfusion still has a role in treatment.
- Dr Iain Cameron was Regius Professor from 1993-2001. His main interests were in reproductive endocrinology and investigation of the impact of the maternal environment on early pregnancy and development. He was appointed Head of the School of Medicine in the University of Southampton in 1994.
- Ian Greer was appointed Regius Professor 2001-2006, transferring from the Muirhead Chair see above).
- Dr Jane Norman was appointed the final Regius Professor in 2006. She performed clinical trials of oral abortofacients, and of drugs for preterm labour; and investigated the role of nitric oxide synthase in uterine cervical ageing. She was appointed Professor of Maternal and Fetal Health in the University of Edinburgh in 2006.

Other Professors
- Edith Hillan was Professor of Midwifery (1998-2001) and was responsible for the introduction of the Master of Midwifery degree. She was appointed as Professor in the Faculty of Nursing at the University of Toronto in 2001.
- Fiona Lyall was appointed Professor of Maternal and Fetal Health in 2003. She was interested in placentation and its impact on pregnancy outcome. She retired in 2016.
- Mary Ann Lumsden was appointed Senior Lecturer, and the first female consultant at the Queen Mother’s Hospital in 1993. She became Professor of Medical Education and Gynaecology, and Head of the Academic Unit of Reproductive and Maternal Medicine in 2004. She has a clinical research interest in menstrual disorders and the menopause. Her research interests have included the impact of hormones on vascular function and cardiovascular disease, the incidence of which is very high in Glasgow. She is also interested in the aetiology and treatment of vasomotor symptoms, their relationship with cardiovascular disease, and new treatments. Another interest has been the mechanism and control of the growth of uterine fibroids and their associated symptoms. These occur in up to 70% of women. She has chaired three national committees which developed clinical guidelines on Heavy Menstrual Bleeding, Ectopic Pregnancy and Miscarriage, and Menopause: Investigation and Management. She is currently Senior Vice-president of the Royal College of Obstetricians and Gynaecologists (2016-2019), and President of the International Menopause Society (2016-2018). She was awarded the OBE in 2017.
- Alan Cameron, currently on the NHS staff at the Queen Elizabeth University Hospital, was appointed Professor of Fetal and Maternal Medicine in 2008. He has supported many clinical trials.
- David Barlow trained in Glasgow before appointment to the University of Oxford as Clinical Reader in 1984, then in 1990 as Nuffield Professor of Obstetrics and Gynaecology. His interest was reproductive medicine, and he was Chair of the British Menopause Society and the National Osteoporosis Society, and President of the European Menopause Society. He led on National Clinical Guidelines on osteoporosis (RCP, 1999) and infertility/in vitro fertilisation (NICE, 2003). In 2005, he returned to Glasgow as Executive Dean of Medicine, and as Head of the Faculty of Medicine had overall leadership of the Medical, Nursing and Dental Schools. He retired from that position in 2010 when the University restructuring brought an end to the University’s Faculties. He subsequently served as the first Director of Women’s Health Services in Qatar.
Andrew Calder, Gordon Lowe, Marjorie Allison

