New optical reporting tool for finding IBD in patient samples
Published: 24 February 2026
A new study co-led by the School of Infection & Immunity's Professor Gwo-tzer Ho has identified a highly-specific immune signal of gut inflammation and translated it into a promising non-invasive diagnostic tool for inflammatory bowel disease (IBD).
A new study co-led by the School of Infection & Immunity's Professor Gwo-tzer Ho has identified a highly-specific immune signal of gut inflammation and translated it into a promising non-invasive diagnostic tool for inflammatory bowel disease (IBD).
Working in collaboration with Professor Marc Vendrell and colleagues in the IRR Chemistry Hub at the University of Edinburgh, Professor Ho helped uncover the role of the enzyme granzyme A (GzmA) as a marker of immune-driven intestinal inflammation.
Inflammatory bowel diseases, including Ulcerative colitis and Crohn's disease, are chronic conditions in which the immune system mistakenly attacks the digestive tract, leading to persistent inflammation and tissue damage.
A central driver of this process is the T cell- a type of white blood cell that normally protects against infection. In IBD, however, certain T cells become overactive and target healthy gut tissue.
Diagnosis and monitoring currently rely heavily on invasive and costly procedures such as colonoscopy, often combined with tissue biopsies.
Imaging techniques like MRI and CT scans provide additional information but cannot visualise the gut lining in sufficient detail.
Less invasive stool tests measure general inflammatory markers such as calprotectin, but these markers are not specific to IBD and can rise in other conditions.
In this new study, titled A chemiluminescence assay targeting granzyme A activity for monitoring inflammatory bowel disease and published in nature biomedical engineering, researchers analysed gut biopsies from patients with IBD and discovered significantly elevated levels of the enzyme granzyme A in inflamed tissue compared with non-inflamed areas.
Granzyme A was found to be primarily released by CD8+ 'killer' T cells - immune cells known to drive tissue damage in inflammatory conditions.
The findings suggest that GzmA activity could serve as a precise molecular signature of immune-driven gut inflammation.
Building on this discovery, the team developed the first non-invasive fluorescent reporter designed to measure granzyme A activity directly in stool samples from patients with IBD and healthy controls.
The reporter, developed within the IRR Chemistry Hub, lights up when it detects GzmA activity. When combined with standard faecal calprotectin testing, the new assay improved identification of IBD compared to calprotectin testing alone.
This dual-marker approach provides greater disease specificity while remaining fast and non-invasive, offering clear advantages over current diagnostic pathways.
The study demonstrates how chemistry-led innovation can deliver clinically relevant tools with direct patient benefit.
By enabling more precise measurement of immune activity, optical reporters such as this could support earlier diagnosis, improved disease monitoring, and ultimately more personalised treatment strategies for patients with IBD.
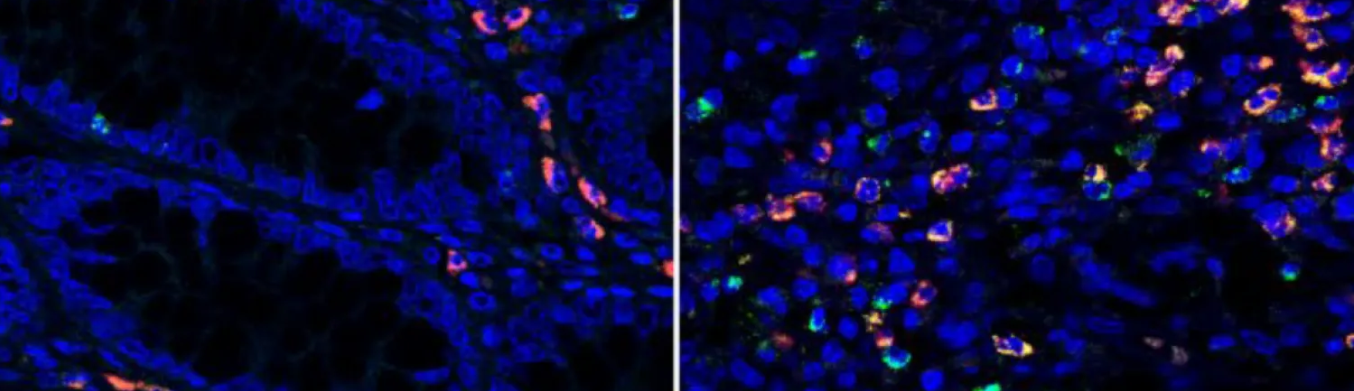
Imaged legend: Microscopy images of colon tissue samples of IBD patients under remission (left) and with active disease (right). Granzyme A (green fluorescence) is elevated in the intestinal tract of IBD patients (right). Credit: Emily Thompson.
Microscopy Images Credit: Emily Thompson
First published: 24 February 2026

