
Study Processes
Figure 1 - Study Management Structure
Figure 2 - Coproduction Process
UKRI ESRC (UK Research and Innovation, Economic and Social Research Council) is the funder of the Partnership for Change Study. Building on our feasibility work (funded by What Works for Children's Social Care) we aim to reduce place-based inequalities by conducting an adaptive Randomised Controlled Trial (RCT) of Infant Parent Support (IPS), with embedded participatory systems mapping and processes evaluation in contrasting UK sites.
The Partnership for Change team includes researchers from the University of Glasgow, the University of Royal Holloway; and practitioners and development leads from the NSPCC.
Background
In 2019/20, UK referrals to child mental health services rose by 35%, yet access to treatment only rose by 4%. Children with psychiatric diagnoses incur more than four times in health and social care costs than their peers. If placed in care, these costs multiple. Providing support sooner is right for the child, family and society. Many children with a social worker and their parents, many of whom may have experienced challenges in their own childhoods or have neurodevelopmental conditions like ADHD or Autism. These families inevitably experience stress, often exacerbated by money or housing problems, and the stigma of living in poverty. This strains relationships and can lead to child maltreatment and children's mental health problems that, in turn, burden families, services and society. Our literature review found no trial evidence for programmes aiming to prevent child maltreatment. However, relationship-focused interventions show promise, especially if involving child protection services. Health and social care organisations, and governments, believe organisations should work together to support families before children are taken into care. A study of an intervention incorporating these elements is timely in this encouraging current policy landscape.
Vision and Approach:
Through our parent-practitioner-community (PPC) partnership developed in the feasibility phase, we have coproduced Infant Parent Support teams (IPS), in Glasgow and London to offer mental health support to struggling families whose children are supported by social work services. In the definitive RCT we plan to further develop the place-sensitivity of IPS teams and test the clinical and cost-effectiveness of IPS in a definitive randomised controlled trial (RCT). The trial will aim to recruit families who have family support services, to explore an early intervention approach.
Placed-based inequalities in health begin early in childhood: young children experiencing poverty and/or racism are much more likely to develop physical and mental health problems earlier in the lifespan than their peers. Children in the most deprived 10% of small UK neighbourhoods are over 10 times more likely to be in care or on protection plans than children in the least deprived 10%. These social determinants of health and child welfare are "systemic, population-based, cyclical and intergenerational" resulting in certain geographical areas being plagued by overlapping physical and mental health problems and additions across generations. Infants and preschool children rely on parents and practitioners to become "candidates" for health and care services - a process vulnerable to structural inequalities. Our novel aim is to redress this.
IPS teams (NSPCC based) offer high quality relationship focused interventions to struggling families. Our coproduction has led to enhancements, including neurodevelopmental awareness, poverty awareness, and the employment of parents with children involved with social work as practitioners and managers in IPS. We have mapped the local contexts in which the IPS teams are embedded, created strong multi-agency partnerships, and involved key stakeholders in our PPC-partnership.
This study consists of four work packages (WPs). We aim to reduce place-based inequalities through: WP1, co-creating a new theory of change for IPS that takes the local context in which IPS tems are embedded into account; WP2,implementing findings from our f-RCT and WP1 to make IPS teams "place-sensitive", i.e., further embedding IPS tems within their local communities and enhancing each local community's ability to make best use of IPS; WP3, examining clinical and cost-effectiveness of IPS in reducing the risk of child maltreatment through a definitive RCT of IPS; and WP4, conducting a realist process evaluation examining what works best, for whom and in what context. RCT outcomes will also include child and parent mental health and community connectedness. At key adaptation points during the RCT, all four WPs will work with an expert scientific advisory group and the PPC-partnership to examine whether we are reaching our desired target population (including marginalised families) and, if not, to enhance our recruitment strategy to achieve equality of access to the study by employing recruiters who come from or have links with under-served populations, and/or targeting specific geographical areas through our extensive networks across Greater Glasgow and in ten diverse London Boroughs. Our success in reducing place-based inequalities will be measured by whether our RCT has recruited a trial population that demographically mirrors our target population. The techniques most successful in achieving this will inform recommendations for post-trial implementation of IPS to ensure the future IPS teams can reduce place-based inequalities by embedding optimally within their local community/service context, and targeting the families likely to most benefit.
Timelines:
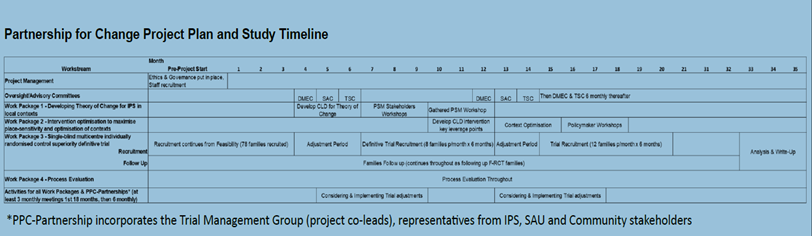
Dissemination:
Supported by our PPI groups, our bespoke dissemination output creation and sharing will strengthen understanding and change practice, supporting implementation of early years mental health findings by practitioners, policy makers, academics, the public, participants and wider stakeholders. It will include peer reviewed publications and wider stakeholders. It will include peer reviewed publications, podcasts, case studies, articles and professional focused briefings.

