Low cost diagnostics for infectious disease elimination
Origami diagnostic tests to aid disease elimination
Infectious diseases bring disproportionate amounts of illness and disability to the poorest and most vulnerable communities in the world. They infect many millions of people but they affect many millions more, with families and communities caught in a cycle of disease and poverty, leading to reduced economic development. Communities within Sub-Saharan Africa carry much of this burden.
Reducing the impact of diseases such as malaria, sleeping sickness, schistosomiasis and rabies is a global priority. Many agencies are working together on ambitious programs to try and eliminate them during the next decade.
To succeed there is a need to monitor hot spots where diseases are prone to re-emerging. This involves screening communities that might carry reservoirs of infection, but with no clinical symptoms.
As part of this monitoring process, there is a need for very sensitive diagnostic tools that can test for multiple pathogens from a single sample. This is called multiplexing. In practice, this means that, when testing for an endemic disease such as malaria, other sensors integrated in the same device can monitor and inform the progress towards elimination of another disease (or multiple diseases).
Such sensors must also be low cost and easily used by healthcare workers to test entire communities that are at risk to re-emergence, following interventions.
With funding from EPSRC ISF, Professor Jon Cooper and colleagues from the School of Engineering, including Dr Julien Reboud and Alice Garret, have been developing a low-cost paper-based diagnostic device to meet these criteria. Crucially, this test can quantify levels of infection using DNA. This provides species-specific information that quickly and accurately informs the appropriate treatment of the infection.
The advantages of DNA-based testing
DNA-based testing comes with many advantages over conventional immunodiagnosis (the detection of antigens and antibodies in the blood or serum). For example, the ability to differentiate between current and historical infections means that the sensors can also quantify the decrease in prevalence within a community. This is crucial to monitoring the progress of a local or national elimination strategy.
DNA-based testing is very sensitive and can also detect asymptomatic levels of infection. This enables the treatment of individuals who appear healthy but have the potential to infect others.
DNA testing has the potential to inform therapy. When more than one species of microbe is co-endemic, a multiplex DNA sensor can provide species-specific information. In malaria diagnostics, for example, effective treatment may depend on this information. Similarly, as the global threat of antimicrobial resistance continues, the ability to detect the drug resistance status and directly inform treatment will become ever more important.
The advantages of paper-based tests
Paper is not only low cost, but it can support predictable microfluidic flows of samples and reagents. It is also easily disposable by burning. Importantly it is one of the few materials with the characteristic to crease and stay creased. Folding paper in a manner similar to origami can bring reagents and samples together and can be used as an easy way of performing sample preparation and washing steps.
Flow of samples and reagents in the paper can be readily controlled using “channels” created by printing hydrophobic layers into the paper. This cheap method for device fabrication, using commercially available hot-wax printing, should enable the production of these tests in the countries where the disease elimination initiatives are taking place.
“Our Biomedical Engineering group at Glasgow has a history of technological innovation and expertise in biosensor technology. Being able to define and control the chemistries of paper using hot wax printing was really an enabling technology in this process.” says Professor Jon Cooper.
Current projects
The paper-based diagnostic platform is currently being adapted and trialled in a number of settings:
Vietnam
This project will develop a new testing platform for the rapid diagnosis of the blood-borne condition sepsis. It is to be used in low-resource areas of Vietnam, where access to infrastructure, equipment and technical expertise is challenging.
The Royal Academy of Engineering will provide £53,000 in support as part of their Frontiers of Engineering for Development programme.
Sepsis is an acute condition arising from an infection which causes the body to damage its own organs and tissues and is often fatal. Around 300,000 patients are affected by sepsis each year in Vietnam, leading to 50,000 deaths annually.
The University of Glasgow’s team, led by Dr Julien Reboud, Dr Melanie Jimenez and Dr Zhugen Yang, will work closely with Dr. Trung Ngo Nat from the 108 Military Hospital in Hanoi, Vietnam, to demonstrate the effectiveness of low-cost, easy-to-use paper ‘origami’ platform which can process large volumes of blood to detect sepsis.
Uganda
This project aims to develop a new health information management system in Uganda. Data from origami diagnosis tests performed in the field will be fed into the national online system for highly prevalent diseases such as malaria and schistosomiasis.
Malaria is the leading cause of death for children under five years of age in sub-Saharan Africa, while schistosomiasis infects 100 million people. The combined effect of these diseases is to help perpetuate a cycle of poverty, illness and mortality, with significant economic impact.
That impact has been mitigated to some extent by strategies to decrease infection rates, such as insecticide-impregnated nets, together with available medical treatment, but the reduction in infections has stalled in recent years.
The University of Glasgow team will work with researchers from Ona, a social enterprise whose mission is to ensure equitable access to services for those who need them most, together with researchers from Makerere University in Uganda.
Ona Co-Founder, Peter Lubell-Doughtie said: “We’re excited to work together on this project. Collaborations between biomedical and computer scientists are essential to accelerate the adoption of life saving innovations like the origami platform.”
Together, the researchers will develop a web-based surveillance platform, using the new low-cost, easy-to-use and connected paper origami molecular diagnostic device to rapidly identify infections in rural communities, enabling faster treatment and adaptation of local interventions.

The architecture of our multiplex device.
Field testing multiplexed origami malaria sensors in Uganda
By Professor Jon Cooper
After initial development and testing in the malaria reference laboratory at The London School of Hygiene and Tropical Medicine, we undertook field tests for a multiplexed, species-specific paper test in Uganda.
Testing can be performed by a non-expert and involves paper-folding to bring the sample and reagents into contact. We integrated the vertical flow (folded) sample preparation with a lateral flow device – akin to a conventional pregnancy test, so that untrained staff could read the test readily. The appearance of coloured lines indicating a positive result.
We tested our devices in Mayuge district, on the banks of Lake Victoria, working with technicians and healthcare workers from Uganda’s Ministry of Health. Prior to testing, a detailed local census was carried out and consent from parents to test children was obtained. Detailed ethical consent, including treatment post-testing was obtained from the ministry.
The study enabled us to take a successfully lab-proven malaria test and explore its deployment into a rural population. As a first preliminary study on a limited number of samples, we were greatly encouraged. Our DNA-based test on a paper platform produced results that were 98.2% accurate, which compared very favourably with immunodiagnostics (82%) and microscopy (86%).
Our field studies informed innovations to improve performance and assay robustness. When doing multiple tests in the same village, over many days, we learnt techniques to mitigate against cross-contamination. We have plans to better interface the sample with the device. We can also increase the speed of the results by reducing the number of processing steps.
We have also now explored the concept of testing malaria alongside schistosomiasis from a finger-prick blood, as a sentinel test. This device particularly excited both the expert technicians and healthcare workers from the Ministry of Health, who were working with us, who saw the potential for this test to improve treatment and save time and resources.
We are now collaborating with a broad range of partners including NGOs, social scientists, community based organisations, governments to further develop, test and find ways to implement the device for use in these types of disease control interventions.

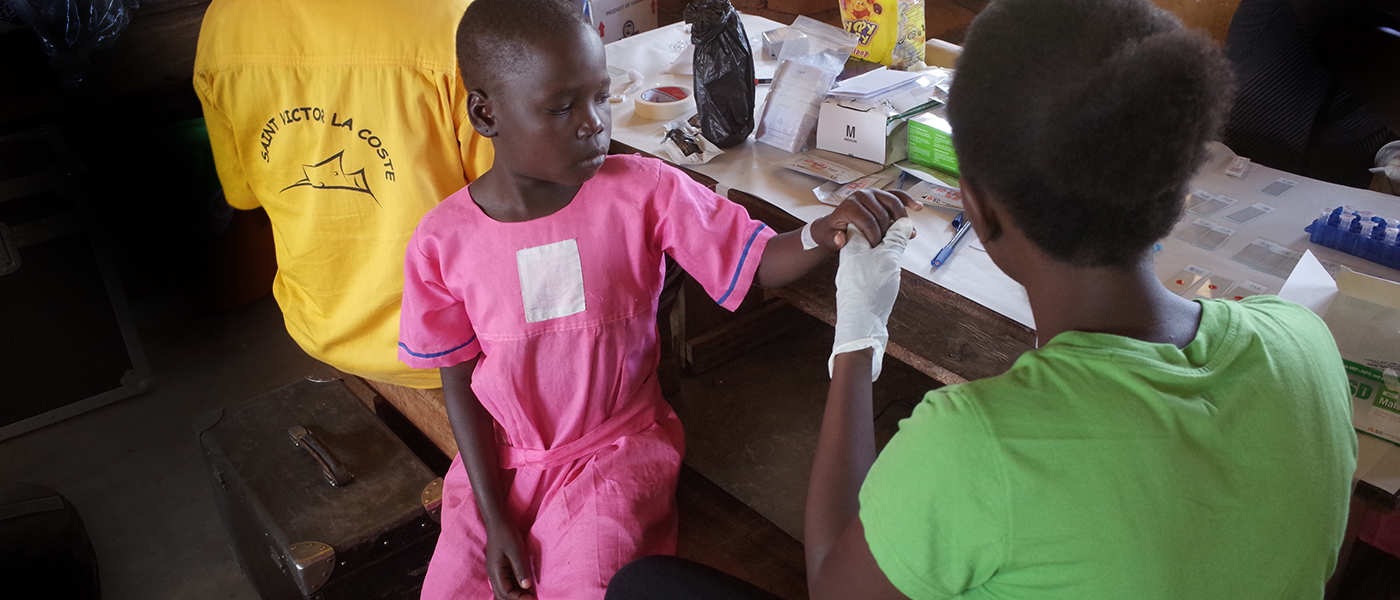
Health worker taking a finger prick blood sample in Mayuge District, Uganda.

